Case Description
A 26 year old female with a past medical history of Hemoglobin SC disease (Hb SC) and iron deficiency anemia presented to the emergency department with lower abdominal pain and diarrhea for three days. She began having multiple episodes of watery diarrhea, followed by bloody diarrhea after eating at a restaurant. During this time, she also had fever, chills, body aches, and headache. The patient had been on a course of ceftriaxone and metronidazole started three weeks prior for sore throat, ear infection, and bacterial vaginosis. She completed her metronidazole course prior to the current illness. Abdominal computed tomography revealed splenomegaly and a mildly dilated, fluid-filled appendix without evidence of infectious or inflammatory abnormalities. Hemoglobin on admission was 11.1 mg/dL (Reference Range: 11.2- 15.7 mg/dL) and MCV 62.9 fL (Reference Range: 79.4- 94.8 fL), which is similar to her baseline.
Laboratory Identification
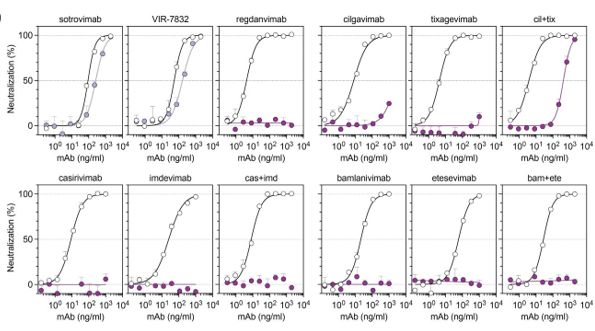
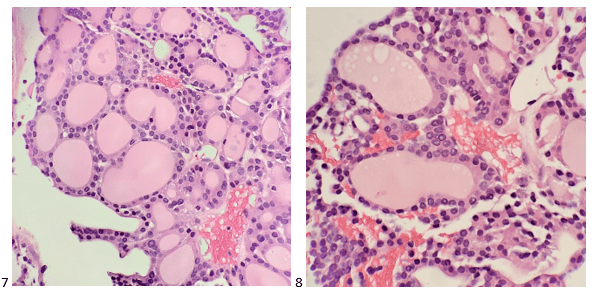
The patient underwent work up for community-acquired diarrhea. Stool cultures grew non-typhoidal Salmonella (Image 1). Blood cultures performed at the time of admission flagged positive with gram negative rods which were also identified as Salmonella species by MALDI-TOF. The organism was susceptible to ampicillin, ceftriaxone, ciprofloxacin, and trimethoprim/sulfamethoxazole. The patient continued on intravenous ceftriaxone and responded to therapy. She was discharged home on oral ciprofloxacin.

Discussion
Hemoglobin SC disease (Hb SC) is the second most common hemoglobinopathy after Sickle Cell Disease (SCD, Hb SS) globally.1 Hb SC disease occurs when a patient inherits both hemoglobin S and hemoglobin C alleles. Hemoglobin S and C variants are caused by point mutations in the hemoglobin beta- chain, and both variants lead to reduced affinity to the alpha-chain. While hemoglobin C is an abnormal form of hemoglobin that does not cause sickling on its own, when co-inherited with hemoglobin S, the beta chains polymerize, causing red cell sickling when oxygen tension is lowered in the blood.2 Patients develop anemia due to reduced red cell lifespan (27-29 days for Hb SC vs. 15-17 days for Hb SS) and subsequent destruction of red blood cells.3
Complications arise from vascular occlusion and destruction of red blood cells, leading to gallstones, pulmonary infarction, priapism, and/or cerebral infarction. Other complications include avascular necrosis of the femoral head, bone marrow necrosis, renal papillary necrosis, retinopathies, splenomegaly, and recurrent pregnancy loss. Although Hb SC patients often exhibit similar symptomology to sickle cell disease, symptoms are typically milder and present later in childhood.2,3 In comparison to patients with Hb SS, Hb SC patients have milder anemia, less frequent sickle cells, and less severe hemolysis. While Hb SC patients have fewer sickling episodes compared to Hb SS patients, Hb SC patients have more severe retinopathy and splenomegaly. It is also important to note that the enlargement of the spleen is often caused by red blood cell sequestration and the optimal function of the spleen is significantly reduced (functional hyposplenia), which can lead to increased risk of infection from encapsulated bacteria.
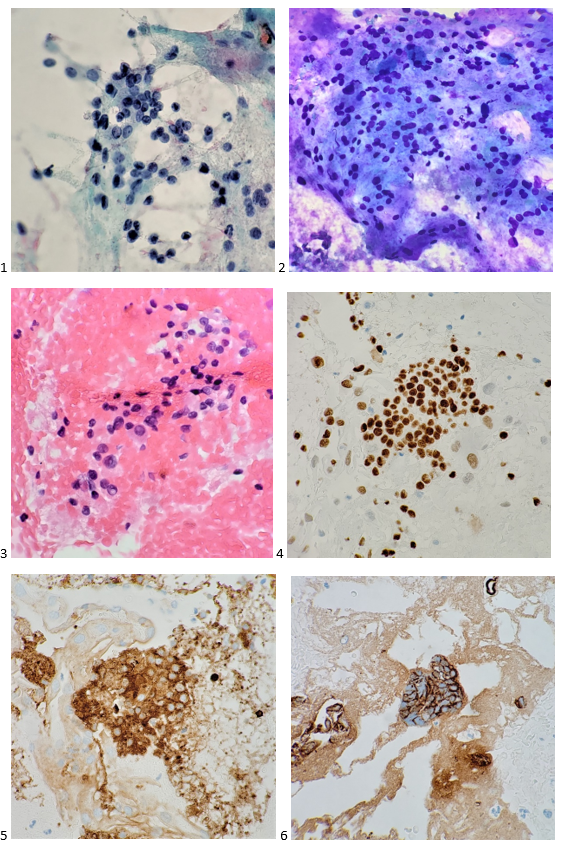
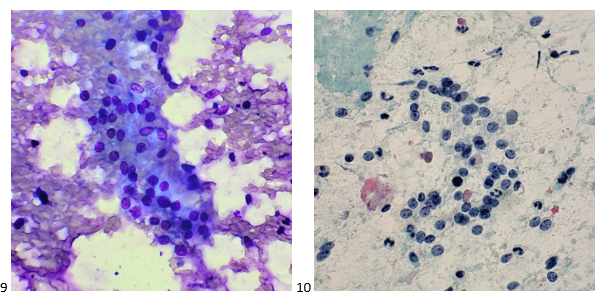
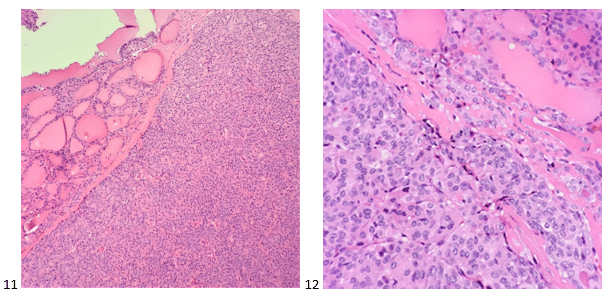
Diagnosis of Hb SC disease is typically made by performing hemoglobin electrophoresis (Image 2). Hemoglobin electrophoresis separates the differing varieties of hemoglobin by size and electrical charge. Capillary electrophoresis separates hemoglobin variants based on the “zone” of detection where each variant hemoglobin appears based on a reference pattern. Normal hemoglobin (A, F, A2) is easily discriminated from variant hemoglobins (S, C, E, D), and quantification allows for detection of beta-thalassemia (increased A2 fraction). While useful as a screening tool, the hemoglobin variants identified in the “zones” are not specific. For example, Hb C and Hb Constant Spring share a zone, and Hb A2 shares a zone with Hb O- Arab. Variants detected by capillary electrophoresis are confirmed by a second method, and in this case Hb SC was confirmed by acid agarose gel (Sebia Hydrogel). When subjected to acid gel electrophoresis, Hb C and Hb S migrate in separate bands, while Hb A, A2, D, and E comigrate in the “A” band, and the “F” band may contain F in addition to the glycated fraction of normal adult Hb A. Patients with Hb SC disease will have variants detected in the S and C zones in capillary electrophoresis and lack signal in the A zone.4

Examination of the peripheral blood smear from a patient with Hb SC disease (Image 2C) reveals frequent target cells, boat-shaped cells (taco shaped), and only rarely contains classic sickle cells. Hemoglobin C crystals can be seen, both free floating and inside red cells, a feature of CC and SC disease but not seen in SS disease. Hemi-ghost cells and cells with irregular membrane contractions are also more frequent in Hb SC disease. In contrast, sickle cells are rarely observed in peripheral smears from Hb SC patients.
Salmonellaeare flagellated gram negative bacilli that are members of the Enterobacterales. Salmonellosis is typically foodborne in nature and presents as a self-limiting acute gastroenteritis.5,6 However, these organisms can invade beyond the gastrointestinal tract resulting in bacteremia.6 This case presents Salmonella as a cause of bacteremia in a patient with Hb SC disease following a bout of gastroenteritis. Although there is a well-known association between SCD and invasive infections with Salmonella, the incidence of Salmonella infection in patients with Hb SC disease has not been well studied. Patients with SCD, particularly those in Africa, are at risk for developing invasive disease caused by non-typhoidal Salmonella, including osteomyelitis, meningitis, and bacteremia. It has been hypothesized that disruptions in the gut microbiome and increased permeability of enterocytes makes SCD patients more prone to invasive Salmonella infections.6 Furthermore, the compromised function of the spleen in both patients with SCD and Hb SC disease increases the risk of disseminated infection by encapsulated bacteria and Gram negative rods. The spleen plays an important housekeeping role removing old or damaged erythrocytes, but also has an important immunological function housing memory B cells, producing antibodies and macrophages that phagocytize circulating bacteria, particulates or other debris and then present the antigens to other immunological cells in the spleen.7 Although sepsis caused by Salmonella is an occasional progression of gastroenteritis, this patient’s Hb SC disease likely increased the likelihood of bacteremia because of her functional asplenia.
References
- Weatherall DJ. The inherited diseases of hemoglobin are an emerging global health burden. Blood. 2010;115(22):4331–6.
- Tim R. Randolph,24 – Hemoglobinopathies (structural defects in hemoglobin),Editor(s): Elaine M. Keohane, Catherine N. Otto, Jeanine M. Walenga,Rodak’s Hematology (Sixth Edition), Elsevier, 2020, Pages 394-423, ISBN 9780323530453, https://doi.org/10.1016/B978-0-323-53045-3.00033-7.
- (https://www.sciencedirect.com/science/article/pii/B9780323530453000337)
- Nathan, D. G., Orkin, S. H., & Oski, F. A. (2015). Sickle Cell Disease. In Nathan and Oski’s hematology and oncology of infancy and childhood (8th ed., pp. 675-714). Philadelphia, PA: Elsevier. Retrieved from https://www.clinicalkey.com/#!/content/book/3-s2.0-B9781455754144000206y.com/#!/content/book/3-s2.0-B9781455754144000206. Accessed 2022.
- Bain, BJ. (2020) Haemoglobinopathy Diagnosis, Third Edition. Hoboken: John Wiley and Sons, Ltd
- Kurtz, J. R., Goggins, J. A., & McLachlan, J. B. (2017). Salmonella infection: Interplay between the bacteria and host immune system. Immunology letters, 190, 42–50. https://doi.org/10.1016/j.imlet.2017.07.006
- Lim, S.H., Methé, B.A., Knoll, B.M. et al. Invasive non-typhoidal Salmonella in sickle cell disease in Africa: is increased gut permeability the missing link?. J Transl Med 16, 239 (2018). https://doi.org/10.1186/s12967-018-1622-4
- Leone G, Pizzigallo E. Bacterial Infections Following Splenectomy for Malignant and Nonmalignant Hematologic Diseases. Mediterr J Hematol
-John Stack is a first year AP/CP resident at UT Southwestern Medical Center.
-Marisa Juntilla is an Assistant Professor in the Department of Pathology at UT Southwestern Medical Center. Dr. Juntilla is a board certified Clinical Pathologist and is certified in the subspecialty of Hematopathology.
-Dominick Cavuoti is a Professor in the Department of Pathology at UT Southwestern Medical Center. Dr. Cavuoti is a board certified AP/CP who is a practicing Clinical Microbiologist, Infectious Disease pathologist and Cytopathologist.

-Andrew Clark, PhD, D(ABMM) is an Assistant Professor at UT Southwestern Medical Center in the Department of Pathology, and Associate Director of the Clements University Hospital microbiology laboratory. He completed a CPEP-accredited postdoctoral fellowship in Medical and Public Health Microbiology at National Institutes of Health, and is interested in antimicrobial susceptibility and anaerobe pathophysiology.

-Clare McCormick-Baw, MD, PhD is an Assistant Professor of Clinical Microbiology at UT Southwestern in Dallas, Texas. She has a passion for teaching about laboratory medicine in general and the best uses of the microbiology lab in particular.