A 72 year old female originally presented with lung carcinoid and bilateral renal masses. The patient’s left kidney biopsy demonstrated ectopic thyroid parenchyma by an outside institution. Her thyroid function tests were unremarkable, she had no known previous head and neck radiation, and to the best of her knowledge, there was no family history of thyroid cancer. She underwent FDG PET imaging, which showed increased bilateral uptake in the neck (thyroid and lymph nodes), and an avid right posterior renal mass. Otherwise, her scan was relatively clear. Her left renal mass was resected and demonstrated thyroid parenchyma, but the differential diagnoses included thyroid heterotopia and metastatic well-differentiated thyroid carcinoma.
FNA and core biopsy were then obtained from the right upper quadrant of the kidney. The findings are depicted below.
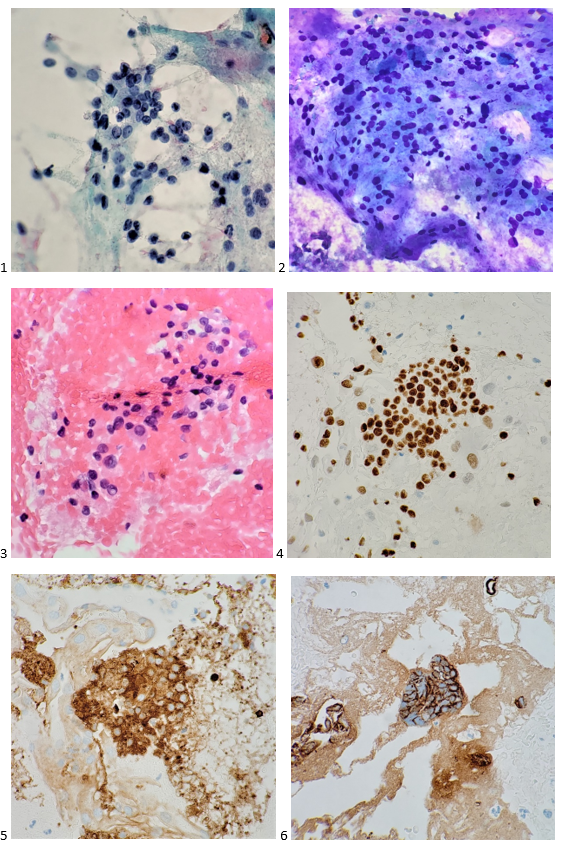
The FNA was signed out as “Atypical thyroid tissue present.” Immunohistochemical stains demonstrated positive staining for CK7, vimentin (partial), TTF-1, thyroglobulin, and PAX-8 (partial), and negative staining for RCC, Napsin A, synaptophysin, and chromogranin. While these immunostains suggest thyroid-type tissue, morphology was most worrisome for metastatic thyroid carcinoma. The chromatin presented as hypochromatic and powdery, nuclear grooves and pseudoinclusions were present, and the nuclei were enlarged with irregular membranes. However, the scant material present precluded a definitive diagnosis.
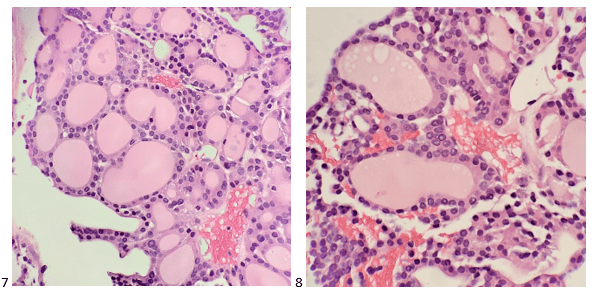
The core biopsy suggested benign-appearing thyroid tissue similar to that seen in the left kidney, however, the surgical pathologist diagnosed the material as metastatic thyroid carcinoma.
A thyroid FNA was obtained from one of the patient’s multiple right-lobed thyroid nodules consistent with TI-RADS category 5 the next day. This was diagnosed as atypia of underdetermined significance due to scant cellularity.
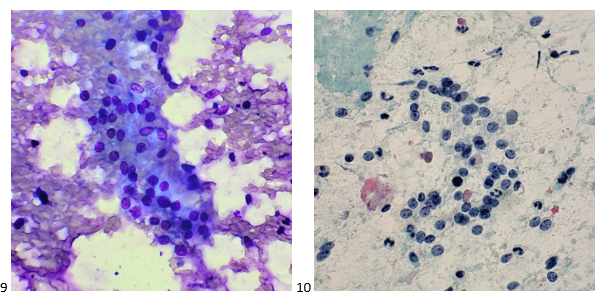
The right renal mass was resected after molecular profiling was performed on the left renal mass tissue. Mutation Detection by Next Generation Sequencing demonstrated a tumor mutation burden of 3.6Muts/Mb and identified mutations in the PRKDC, PTEN, and KRAS genes. Two kidney tumors were identified in the right kidney (one measuring 8.0 cm and the other 4.5 cm), both diagnosed as metastatic thyroid carcinoma with papillary features.
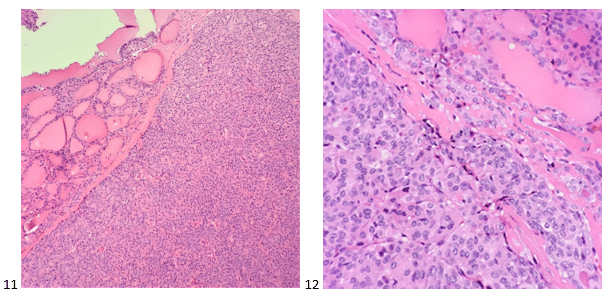
The thyroid was then resected, and pathologic findings were consistent with invasive follicular carcinoma with extensive angioinvasion to 4 or more vessels. While renal metastases are rare, the high affinity for angioinvasion makes the kidney a prime metastasis site due to its vascular-rich tissue. The patient was prescribed a low iodine diet and Thyrogen-stimulated radioiodine ablation to remove any remaining thyroid tissue or micrometastases and enhance the sensitivity of thyroglobulin as a tumor marker for surveillance purposes. While thyroid cancer (papillary and follicular types) is typically considered “the best cancer to have” due its slow growth and low-risk of widespread malignancy, it doesn’t mean that it won’t metastasize, even to a distant organ that you normally wouldn’t suspect. Great caution must be taken to ensure that lumps, bumps, and swallowing issues are addressed at annual physicals to catch a low-risk cancer before it has the opportunity to become an epic metastasis.

-Taryn Waraksa, MS, SCT(ASCP)CM, CT(IAC), has worked as a cytotechnologist at Fox Chase Cancer Center, in Philadelphia, Pennsylvania, since earning her master’s degree from Thomas Jefferson University in 2014. She is an ASCP board-certified Specialist in Cytotechnology with an additional certification by the International Academy of Cytology (IAC). She is also a 2020 ASCP 40 Under Forty Honoree.
