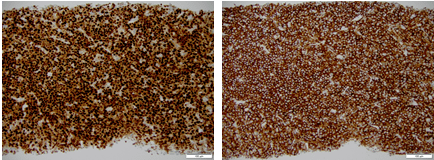
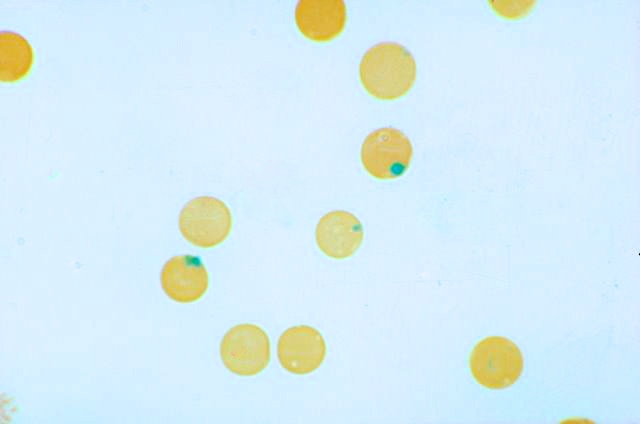
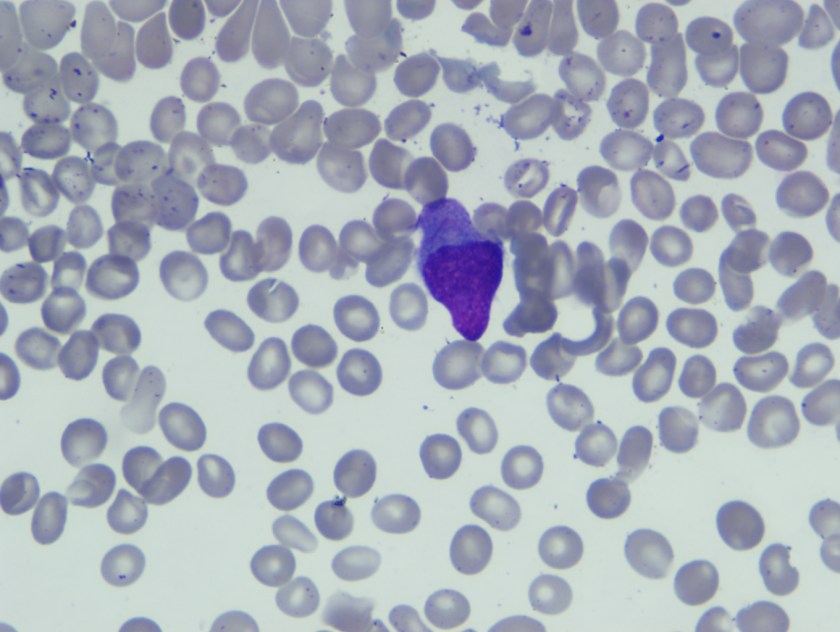
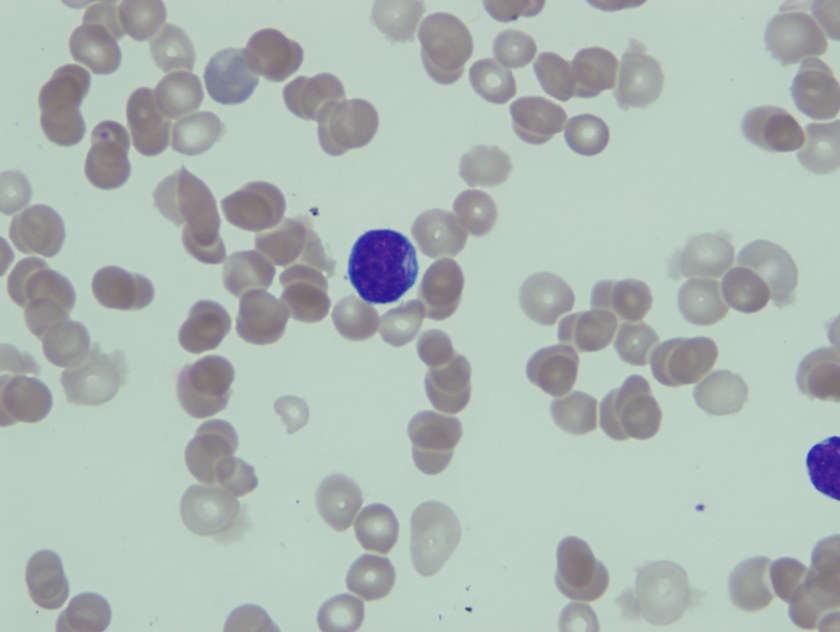
Sickle cell disease is a blood cell disorder that affects a lot of Americans, especially those of African descent. The disease is a result of a genetic defect that changes the structure of hemoglobin. This alteration in hemoglobin causes normally round red cells to become sickle in shape as well as sticky and deformed. As a result, these deformed red cells block perfusion of red blood cells into circulation and vital organs and affects the vasculature resulting in severe pain, organ damage and sometimes stroke.
Management of sickle cell disease includes blood transfusion, hydorxyurea and pain management. The long-term administration of hydroxyurea to stimulate the production of fetal hemoglobin is a form of therapy that provides relief in that fetal hemoglobin essentially protects the red cells from sickling. The transfusion of red cells lowers the amount of sickle hemoglobin levels.
Transplantation of hematopoietic stem cells from HLA-identical siblings can be curative in several nonmalignant hematologic disorders, including aplastic anemia, β-thalassemia major, congenital immunodeficiency disorders, and certain inborn errors of metabolism. Pilot studies of bone marrow transplantation for the treatment of young patients with symptomatic sickle cell disease have demonstrated eradication of the underlying disease with low transplantation-related mortality (Bhatia and Walters, 2007).
The process for successful bone marrow transplant to cure sickle cell involves administration of chemotherapy or immunosuppressive drugs to eradicate all the cells. Now, doctors have developed a more successful regimen where patients take immunosuppressive drugs with a low dose body irradiation, a treatment much less harsh than chemotherapy. Next, donor cells from a healthy and tissue-matched sibling are transfused into the patient. Stem cells from the donor produce healthy new blood cells in the patient, eventually in sufficient quantity to eliminate symptoms. In many cases, sickle cells can no longer be detected. Patients must continue to take immunosuppressant drugs for at least a year.
In the reported trial, published online in the journal Biology of Blood & Marrow Transplantation, physicians from the University in Illinois Chicago transplanted 13 patients, 17 to 40 years of age, with a stem cell preparation from the blood of a tissue-matched sibling. In a further advance of the NIH procedure, the physicians successfully transplanted two patients with cells from siblings who matched but had a different blood type (Parmet, 2015)
Stem cell transplantation has proven itself to provide cures for a lot of hematologic malignancies, now it is successfully finding its way to cure other hematologic abnormalities, including sickle cell anemia. This continued advancement in medicine will provide relief to a lot of patients who are suffering from sickle cell disease.
References
- Bhatia, M., & Walters, M. C. (2007). Hematopoietic cell transplantation for thalassemia and sickle cell disease: past, present and future. Bone Marrow Transplantation, 41(2), 109-117. doi:10.1038/sj.bmt.1705943
- Parmet, S. (2015). Adults with sickle cell disease cured with stem cell transplants. Retrieved March 25,2017, from https://news.uic.edu/cure-for-sickle-cell

-Carlo Ledesma, MS, SH(ASCP)CM MT(ASCPi) MT(AMT) is the program director for the Medical Laboratory Technology and Phlebotomy at Rose State College in Midwest City, Oklahoma as well as a technical consultant for Royal Laboratory Services. Carlo has worked in several areas of the laboratory including microbiology and hematology before becoming a laboratory manager and program director.