Hello everyone and welcome back!
Last month, it was as fun to write about hematology peripheral smear differentials as it was to address the importance of interdisciplinary collaboration. I found myself in a unique position both as a medical student as well as a former medical laboratory scientist in what was a great clinical training rotation in hematology/oncology. Now, with just one rotation left until the end of my medical school journey, I want to take you on a look back at some of the very first posts I made here on Lablogatory and update you on the intersectional, collaborative topic that I shared with you almost two years ago: Zika!

In a recent digital article on ASCP’s partner, The Pathologist, author and staff editor Michael Schubert wrote about the connectivity between public health, epidemiologic research, laboratory medicine, and clinical patient outcomes. He examined the effectiveness and accuracy of Zika testing availability in commercially available assays and spoke with a leading virologist in the field from Berlin. You may recall one of those “ancient” posts I made about Zika, where I was part of a research team that used the same methodology! Combined immunoglobulin-specific assays, arbovirus detection in the heat of a public health epidemic’s epicenter, and lab medicine that complimented my concurrent immunology class in med school—what more could you ask for?
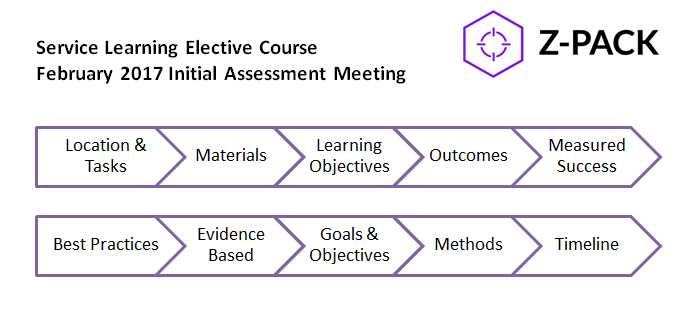
And, since the last tagged Lablogatory Zika update I can see was by Dr. Sarah Riley in February of 2017, here’s my update! Dr. Riley’s post was a fantastic summary of the Zika epidemic, its troublesome diagnostic assessments, and the recommendations and plans of organizations like the World Health Organization (WHO). She was, and still is, right—the “struggle is still real’ when it comes to Zika testing. Curious about what it was like during the 2016 epidemic? Who was doing testing, what kind of testing, and what was the lab data climate? Well…it feels like it’s time for a…
*** FLASHBACK ***
An Arbovirus Abroad
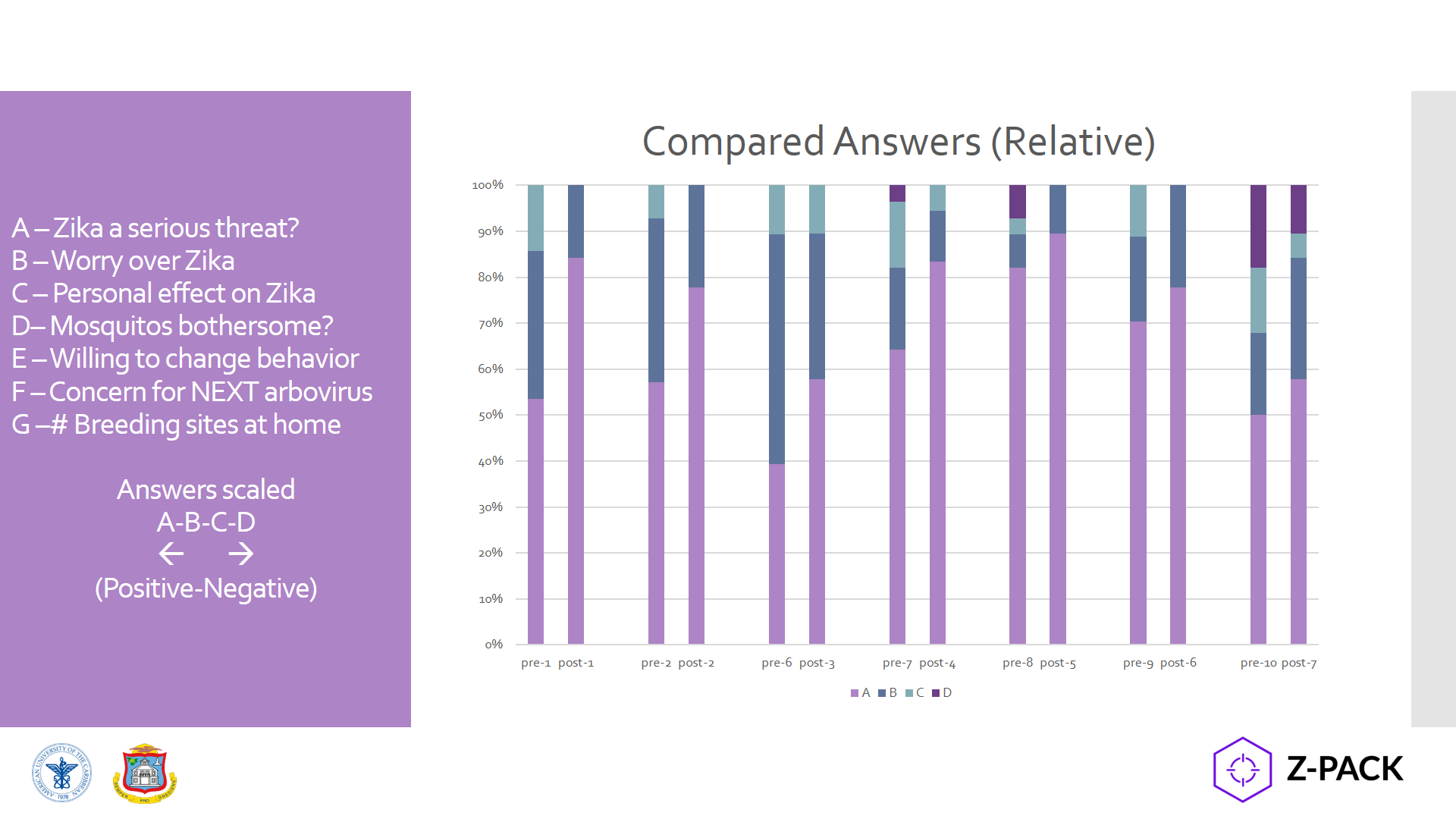
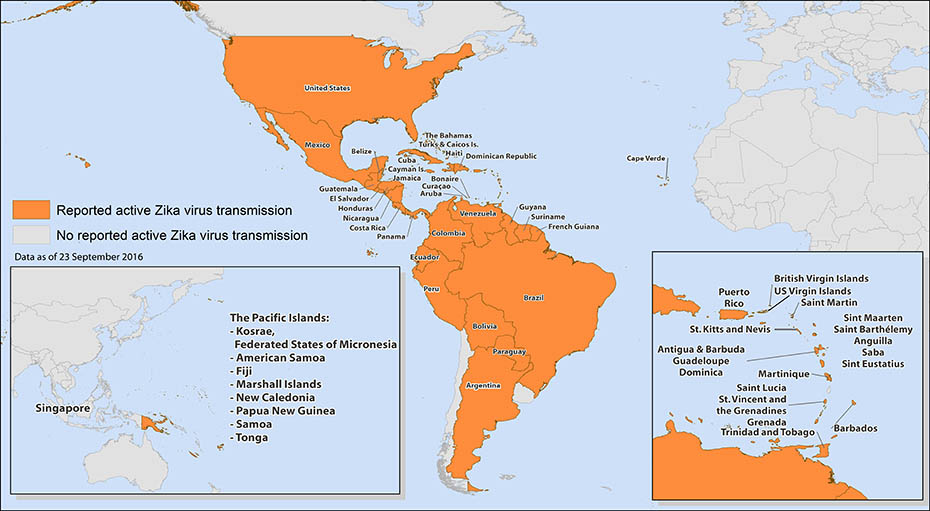
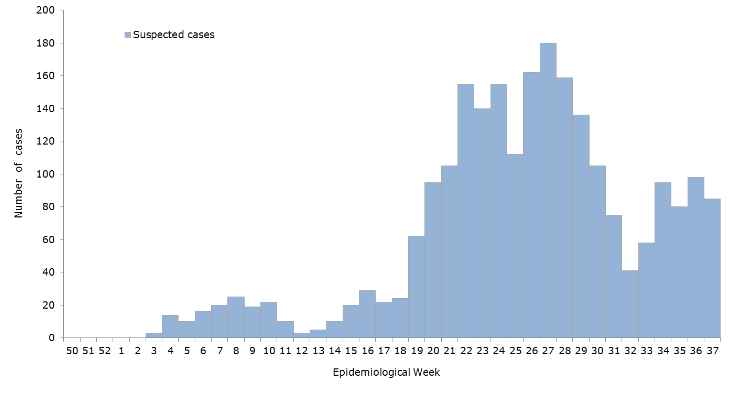
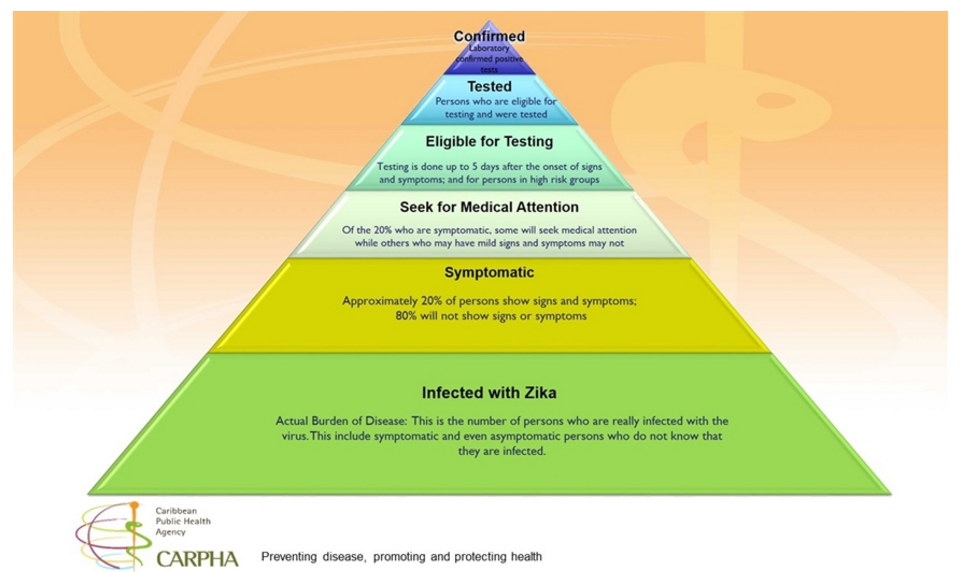
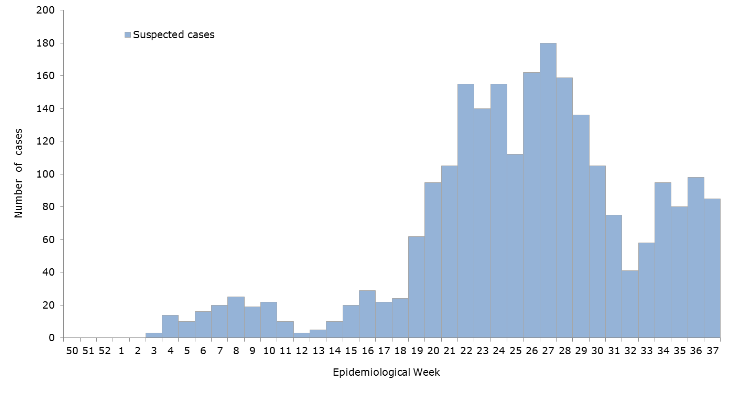
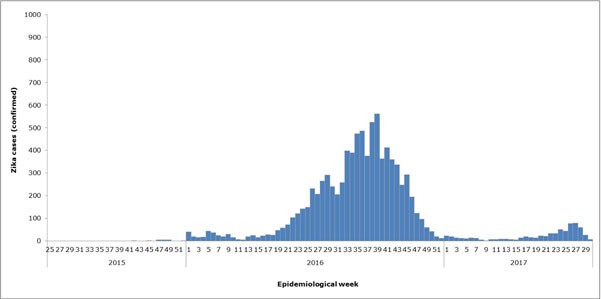
Hey! My inaugural post! It was fun to go back and see the data from the work then (Spoilers: epidemiologic updates are on your horizon). We were just getting started to take an assessment of the situation and address it as a public health concern. My then Caribbean location was a great place to study Zika trends coming from Brazil, Puerto Rico, and Florida. As a snapshot, at that time (Dec 2016) there were a purported almost 2,000 cases, however less than a fifth of those cases were serologically confirmed by lab testing. Before the recommendations to move toward RT-PCR, most labs in the region were requesting commercially available screening tests for IgG/IgM assays.
Healthy Me
How do you reach people when you’ve got compelling public health lab data that translates to possible prevention of infection and spread of disease? Easy: go to where the people are and engage them when and where they’re comfortable. One of the overarching themes in public health is mitigating barriers to change by way of utilizing social humility. This a certainly a type of interdisciplinary collaboration because if we’re the experts on IgM and IgG trends in testing confirmations, the public are the experts in social determinants of health within their communities.

Laboratory Data and Global Health Security
As my team and I were busy preparing SOPs, conducting a new project aimed at improving local health literacy and source reduction, securing IRB approval, and collecting data about the residents of Sint Maarten to correlate with local Health Ministry projections, one of the officials—who now serves as a regional director for PAHO—took our work to the Global Health Security Agenda Summit. Talk about motivation! In and out of the lab, I worked with teams who were getting some fantastic work done on the ground with respect to mosquito-borne virus research.

IRBs and Public Heath Pathology
For those of us who work in laboratory medicine, it’s easy to talk about the best way to test, detect, and treat an epidemiologic threat—it’s even exciting when it’s a current threat. But to really be successful, you’ve got to collaborate with those outside of the lab, and often this means thinking “outside the box.” Public health is different from lab medicine in that while lab-work is based around results, testing, and organized data-driven decisions, success in public health is highly determined by community buy-in in the form of partnerships!
*** FLASH … FORWARD? ***
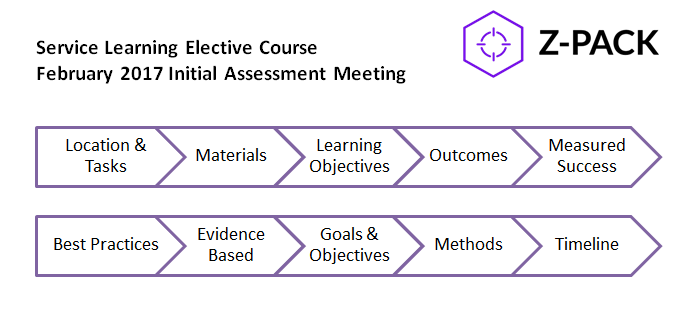
So, after my time in Sint Maarten, I came to New York City to rotate through my clinical clerkships. And, if you’ve seen some more recent post-Zika posts on this website, you know they’ve been going great! Within a few months of being here, my wife brought back some swag from a training session she attended. (Side note: she’s a graduate-level nurse, working in the public health non-profit sector with vulnerable populations in the inner city—she’s too busy to blog.) After months of both of us working and learning about Zika and public health initiatives in the Caribbean, we were greeted by this fantastic toolkit from the New York State Department of Public Health!


The take home message: collaboration is key, both inside and out of the lab. Schubert’s piece in The Pathologist created a fantastic dialogue in addressing the clinical needs for interdisciplinary collaboration. The best testing means finding out exactly where the needs are and using data-driven decisions to implement change or action. In the lab, that means constantly working for higher quality and better patient outcomes in every test, result, report, and (mosquito) byte of data. In the field, it means the same thing, but instead of metrics like sensitivity, specificity, and TAT it’s about cultural humility, attainable goals, and dynamic timing.
Thanks for reading! Hope most of our national heat wave spared you, but if it didn’t remember: don’t keep standing water around, wear light loose clothing, and use appropriate insect repellent!
See you next time!

–Constantine E. Kanakis MSc, MLS (ASCP)CM graduated from Loyola University Chicago with a BS in Molecular Biology and Bioethics and then Rush University with an MS in Medical Laboratory Science. He is currently a medical student actively involved in public health and laboratory medicine, conducting clinicals at Bronx-Care Hospital Center in New York City.