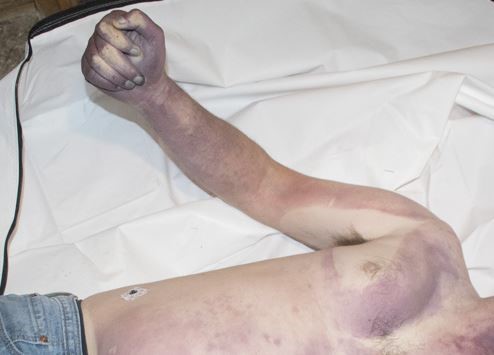
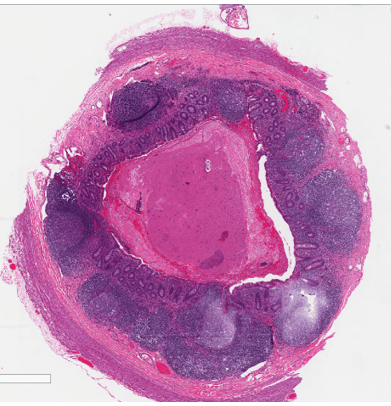
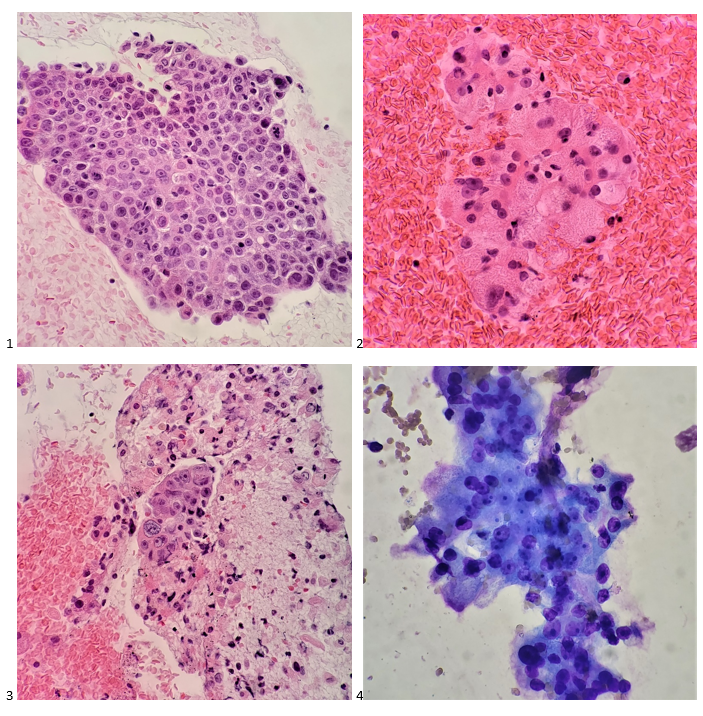
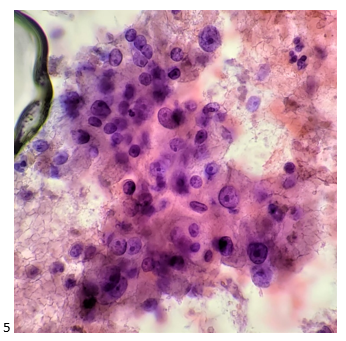
When I perform an autopsy, I know that anything I find will be discovered too late to save my patient’s life. I generally hope the autopsy report helps explain why and how someone died to family members, law enforcement, lawyers, and potential jurors. It’s less common that an autopsy finding can have immediate impact on the healthcare of the decedent’s family, but this is the case with thoracic aortic disease.
Thoracic aortic aneurysms and/or dissections (TAAD) are relatively common mechanisms of sudden, unexpected, and natural death we encounter in forensic pathology. The classic teaching is that TAAD are caused by hypertension, bicuspid aortic valves, pregnancy, and cocaine use. Genetic disease1,2,3 is included late in the list, almost as an afterthought, with Marfan syndrome given as the prototype. However, the evidence for a genetic underpinning of TAAD has been steadily expanding. Family pedigrees in the late 1990s revealed up to 20% of patients with TAAD had an affected first-degree relative.4,5 If extended to 2nd degree relatives, up to 43% of patients with TAAD had at least one affected family member.6 There are also now more than 15 types of defined connective tissue diseases, and more than 29 genes identified which are mutated in heritable TAAD (H-TAAD). Clearly, the etiologies of hereditary TAAD (H-TAAD) expand far beyond Marfan syndrome.
H-TAAD can be categorized as “syndromic” or “non-syndromic” and has wide variability in clinical presentation. Syndromic forms show multisystem involvement, and often have externally apparent phenotypes. The most common forms of syndromic H-TAAD are Marfan syndrome, vascular Ehlers-Danlos, and Loeys-Dietz syndrome. However, the physical appearances associated with these syndromes can be subtle and aren’t always present.7 Non-syndromic H-TAAD affects only the aorta and aortic valve and includes both bicuspid aortic valve-associated TAAD and “familial” H-TAAD.
Thoracic aortic disease often remains subclinical until serious, life-threatening complications occur. Forensic pathologists can therefore play an important role in preventative health, proactively identifying patients at high risk for TAAD. Because a relatively large percentage of thoracic aortic disease is hereditary, it is prudent to ask whether forensic pathologists should initiate genetic testing in these situations. Unfortunately, postmortem genetic testing is still out of reach for most Medical Examiner and Coroner systems. Insurance companies don’t reimburse for postmortem genetic tests, even when requested by healthcare providers of the surviving family. Selective testing of decedents with high-risk features may be more affordable, but there is no consensus on what those “high-risk” features are – and because of the variable penetrance and expressivity of H-TAAD, patients can present at nearly any age (even in their 80s).5,6
Despite the limitations of access to postmortem genetic testing, the most practical resource forensic pathologists have at our disposal is the telephone. According to 2022 guidelines from the American College of Cardiology and American Heart Association, aortic imaging is recommended in all first-degree relatives of patients with TAAD to screen for occult disease.8 Family members therefore need to be notified of this recommendation, regardless of the pathologist’s choice to pursue genetic testing. Developing a collaborative relationship with a local hospital or academic center may be beneficial; medical examiner offices then have a place to refer families for screening, and genetic counselors in these locations are better suited to evaluate the entire family and potentially order targeted genetic tests.9
Forensic pathologists are in a crucial position to recognize potential H-TAAD. Surgical outcomes for patients with TAAD are much better when performed prophylactically rather than emergently, so identifying aortic disease prior to rupture or dissection is crucial. Premature attribution to hypertension, or overreliance on the presence of Marfan-like features to identify hereditary disease, will result in missed opportunities to save lives. Forensic pathologists can therefore have a significant impact on public health, by recognizing the heritability of TAAD and contributing to improved screening of families at risk.
References
- Prahlow JA, Barnard JJ, Milewicz DM. Familial thoracic aortic aneurysms and dissections. J Forensic Sci. 1998 Nov;43(6):1244-1249.
- Gleason T. Heritable disorders predisposing to aortic dissection. Semin Thorac Cardiovasc Surg. 2005 17:274-281.
- Gago-Diaz M, Ramos-Luis E, Zoppis S. Postmortem genetic testing should be recommended in sudden cardiac death cases due to thoracic aortic dissection. Int J Legal Med. 2017 Sep;131(5):1211-1219.
- Biddinger A, Rocklin M, Coselli J, et al. Familial thoracic aortic dilatations and dissections: a case control study. J Vasc Surg. 1997;69:506-511.
- Coady MA, Davies RR, Roberts M, et al. Familial patterns of thoracic aortic aneurysms. Arch Surg. 1999;134:361-367.
- Chou AS, Ma WG, Mok SCM, et al. Do familial aortic dissections tend to occur at the same age? Ann Thorac Surg. 2017 Feb;103(2):546-550.
- Isselbacher EM, Cardenas CLL, Lindsay ME. Hereditary influence in thoracic aortic aneurysm and dissection. 2016. Circulation 133(24):2516-2528.
- Isselbacher EM, Preventza O, Hamilton Black 3rd J, et al. 2022 ACC/AHA Guideline for the diagnosis and management of aortic disease: A report of the American Heart Association/American College of Cardiology Joint Committee on Clinical Practice Guidelines. Circulation. 2022 Nov 2. Online ahead of print.
- Krywanczyk A, Rodriguez ER, Tan CD, Gilson T. Thoracic aortic aneurysm and dissection: Review and recommendations for evaluation. Am J Forensic Med Pathol. 2023 Mar 6.

-Alison Krywanczyk, MD, FASCP, is currently a Deputy Medical Examiner at the Cuyahoga County Medical Examiner’s Office.