Usually, I talk about some of the more administrative happenings in the laboratory world (accreditation, competency, etc.). Today, however, as there is seemingly a glimmer of light at the end of the nation’s pandemic tunnel, I thought I would reflect on what we have collectively experienced.
Like much of the nation, it has been a difficult journey for laboratorians. It has been particularly trying for those who were asked, who were required, to rise up and meet the unprecedented challenges of the times while suffering from the same burdens of fear, uncertainty, and physical ailments as those they were serving.
Dying Alone
One year ago, my uncle died from COVID-19. He died alone and afraid in the nursing home where he never wanted to be. We visited him after being given special permission from the president of the company operating the nursing home. After being told about how unusual it was to be allowed to see him, we dressed in full PPEs and went into his room. We found him curled in a fetal position, dead and cold to the touch. It was so unfair.
I think about all of the laboratorians who had to endure similar or worst experiences: those who lost close family members and even those who themselves suffered through the disease.
Unseen Warriors
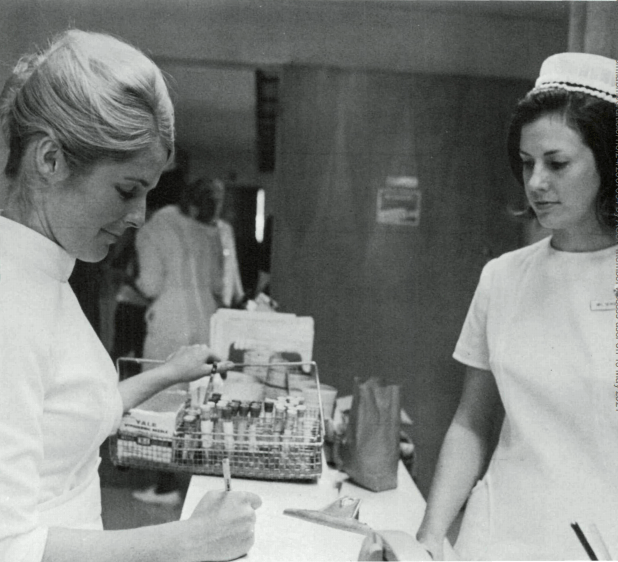
Laboratorians have always been the silent warriors in the life-long battle to defeat pain and disease. More often, nurses and doctors received public gifts of admiration and praise for their service to patients. With quiet satisfaction, laboratory technologists, technicians, and support personnel are dedicated 24 hours a day, seven days a week, to providing the information on which 70% of medical decisions are based. Information that no other group of professionals can provide.
I think about all of the effort and skill required in the mad rush to set up tents and collection sites needed across the nation. And then, too, there were the laboratories needing to scale up testing or create entirely new testing areas with new instruments and new tests kits. The chaos was magnified by constantly changing guidelines, reagent shortages, and a lack of trained personnel.
Amid all the confusion, misinformation, and anger, laboratorians were themselves experiencing disease, death, and social isolation. Yet still, they delivered the results the nation needed to understand the pandemic’s depth and breadth.
Needless Death
Now the Delta variant has taken hold just when the nation thought the disease, if not bested, had at least been brought under some semblance of control. Unfortunately, the refusal of many to get vaccinated contributes to the virus’s persistence. More will suffer, and more will die.
How many needless deaths will the nation have to experience? Will there ever be a point when everyone who can be vaccinated will be? Or, two years later, will we be mourning preventable COVID-19 deaths. Will we still have to watch our loved ones perish with a tube down their throat, or worst, alone in a room far away surrounded by cold walls and quiet indifference?
Sigh.
Regardless of where this pandemic leads or how the nation reacts, laboratorians will continue to remain steadfast in their dedication to their profession and their patients. We have often considered ourselves the stepchild of the healthcare industry because, despite the criticality of what we do, we go unnoticed and unremarked on as long as we deliver the results our patients need. We are okay with that.
We are also tired and worn.
Conclusion
Thanks, fellow laboratorian, for reading this minor soliloquy of frustration and sadness. I will probably be back next quarter discussing inspections, competency, or some other administrative aspect of laboratory operations. I hope, also, to discuss how the nation has reached or is close to reaching the theoretical goal of herd immunity because of high vaccination levels. However, if I were honest, I know the likelihood of this happening is disappointingly low.
If you can get vaccinated, please do.

-Darryl Elzie, PsyD, MHA, MT(ASCP), CQA(ASQ), has been an ASCP Medical Technologist for over 30 years and has been performing CAP inspections for 15+ years. Dr. Elzie provides laboratory quality oversight for four hospitals, one ambulatory care center, and supports laboratory quality initiatives throughout the Sentara Healthcare system.