Diffuse gastric wall thickening has a differential of diffuse inflammatory processes such as peptic, autoimmune disease or Crohn’s gastritis vs. diffusely infiltrative malignancies such as primary carcinoma, metastatic carcinoma or lymphoma by imaging alone.
Whether primary or metastatic, the gastric mucosa may appear relatively normal on endoscopy due to the infiltrative growth (sparing the surface epithelium). Modalities including fluoroscopy and CT scan can aid in assessing wall thickening and give some estimate of gastric distention, as noted in our case.
In our case, following diagnosis on the biopsy, perioperative chemotherapy with 3 cycles of 5-flurouracil, leucovorin, oxaliplatin, and docetaxel (FLOT) was planned. However, after just one cycle, the patient’s clinical course became complicated with severe abdominal pain. A CT scan of the abdomen/pelvis with no intravenous or oral contrast showed a perforated antral ulcer (Image 4 A axial and B sagittal reconstructions, with Red arrows indicating the full thickness gastric wall defect). Findings were confirmed on a water-soluble contrast swallow test (Image 4 C: Blue arrow indicating the ulcer and Red arrow indicating extraluminal contrast layering in the peritoneal cavity). Free intraperitoneal air due to perforation was also evident (Image 4 C: Yellow arrow). Image 4, composite radiographs A-C.
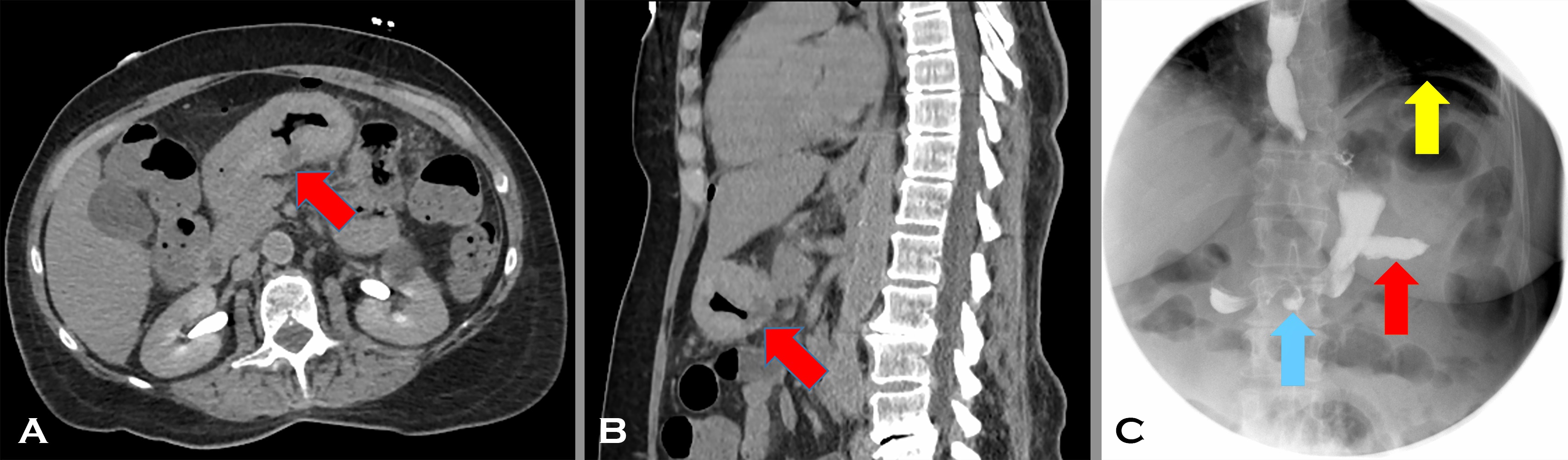
The patient was taken emergently to the operating room and was treated with total gastrectomy, lymph node dissection, Roux-en-Y esophago-jejunostomy and J-tube feeding placement.
The resection specimen had a 1.5 x 1.0 cm perforation in the antral region. Otherwise, there was no discrete lesion or mass. The gastric wall, however, appeared thickened and fibrotic. Lymph nodes were prominent. Microscopic images of the thickened gastric wall are provided below (Image 5, composite photomicrographs A-C). Descriptions of the resection and biopsy micrographs are also included in the discussion below.

What is your diagnosis?
