In the United States, victims of gunshot wounds represent a significant majority of all homicides (and a high proportion of suicides). There’s a propensity among other medical specialties to think of forensic pathologists as “bullet pullers,” just collecting the used projectiles and moving on to the next case. However, autopsies of multiple gunshot wound victims can be some of the most detailed examinations we perform. Even though the cause of death isn’t a mystery, thorough observation and documentation is crucial for other questions which may arise – was the victim immediately incapacitated? Did the shooter reload during the assault? How close to the victim were the shots fired? To address these questions, it’s first helpful to understand the basics of gunshot wounds.
Gunshot wounds can be penetrating (entering the body without exiting) or perforating (entering and exiting the body). Full body x-rays are taken in all gunshot wounds to identify retained projectiles, all of which must be recovered as evidence. It’s important to not use metal tools (like forceps or scissors) when removing a projectile, which may scratch metal and interfere with ballistics comparison.
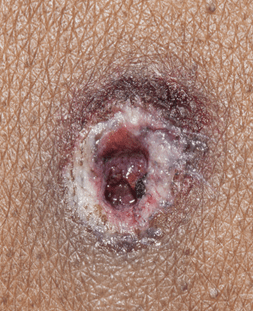
Under typical circumstances, distinguishing entrance from exit wounds is straightforward. Classic entrance wounds are circular, as the bullet hasn’t yet been deformed, and there is a surrounding rim of abrasion where the edges of the bullet scrape against the skin. In contrast, exit wounds have a stellate or slit-like appearance, but the wound edges can typically be reassembled and are not abraded. As with any area of medicine, though, real life doesn’t always follow the rules. An entrance wound can be atypical if the bullet has passed through an ‘intermediary target’ before striking the victim (say a piece of furniture or a car door). If the area of exit is pressed against a firm object (even a tight pants waistband), the skin edges will be abraded (or “shored”). Sometimes, the entrance and exit truly cannot be distinguished – this is more likely with superimposed decomposition, insect activity, or superficial wounds.
Range of fire is another important feature to note and is the reason we always take photographs of a wound before cleaning the body. When a gun is fired, smoke, soot, and unburnt particles of gunpowder exit the barrel as well as the bullet. The smoke creates “fouling,” dark discoloration which easily wipes away and can be seen if the end of the barrel is within approximately one foot of the victim. Stippling, caused by unburnt grains of gunpowder, are actual abrasions and can be seen when the projectile fired within 18” of the victim. These are gross generalizations, though, and in each individual circumstance the weapon itself must be tested to identify the distances. If soot or gunpowder particles aren’t visible on the skin surface, they may have been deposited on the victim’s clothing. ‘‘Bullet wipe’ is slightly different from fouling, in that it is dirt and residue on the actual bullet which gets ‘wiped’ off around the entrance wound on clothing – so it doesn’t tell you range of fire, but it can be helpful to identify tricky entrance wounds.
Now, for some of the common misconceptions around gunshot wounds …
Can you tell the caliber of the gun from the size of the wound? The answer is an emphatic “no.” Much of the injury caused by a bullet comes from the temporary wound cavity created by dissipation of kinetic energy; so no matter the size of the bullet, tissue will stretch and distort around it.
Can you tell the order in which gunshot wounds were sustained? Most often, no. In some autopsies, the first wounds cause so much blood loss that the later wounds lack hemorrhage, but this is the exception rather than the rule.
Can I tell what position the victim was in when they were shot? Again, usually not. In isolation, an autopsy can only tell you the trajectory of the bullet through the body; to determine the position of the victim when they were shot requires knowledge of either where the gun was when it was fired or where the bullet landed–two factors which are often not available.
These are just a few of the complexities faced by a pathologist when working with gunshot wounds, and we haven’t even covered different types of ammunition or firearms. Stay tuned for more in the future!



-Alison Krywanczyk, MD, FASCP, is currently a Deputy Medical Examiner at the Cuyahoga County Medical Examiner’s Office.

