Patient History
A 54 year old woman is seen by her oncologist with complaints of rigors and fevers for the past two months. Her past medical history is significant for Stage IV Follicular Lymphoma. Previous treatment included rituximab and bendamustine that was completed a year prior. Currently her therapeutic plan is to receive rituximab maintenance therapy every two months (her most recent dose was 2 days prior to this visit) via a port. She has two dogs, both of which had a diarrheal illness three months prior. She has chickens and spent the summer RV camping around New England. She has not had diarrhea or noticed any rashes. Her travel history includes a trip to Europe 4 years prior. A blood culture was collected due to her fevers and rigors and was found to be positive 29 hours post incubation.
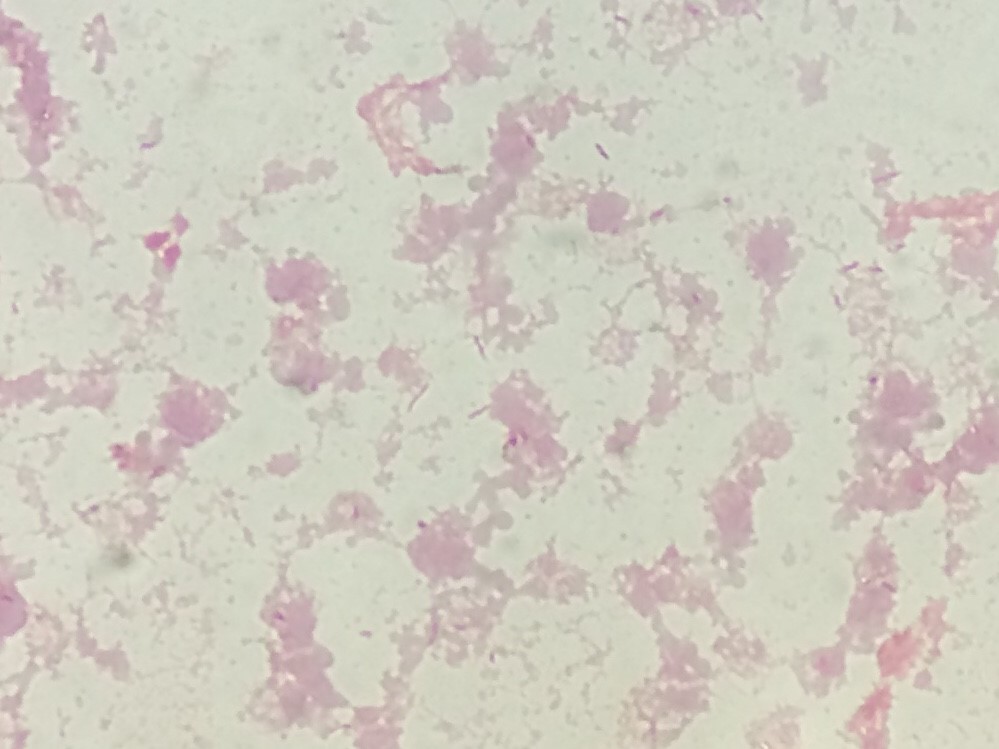
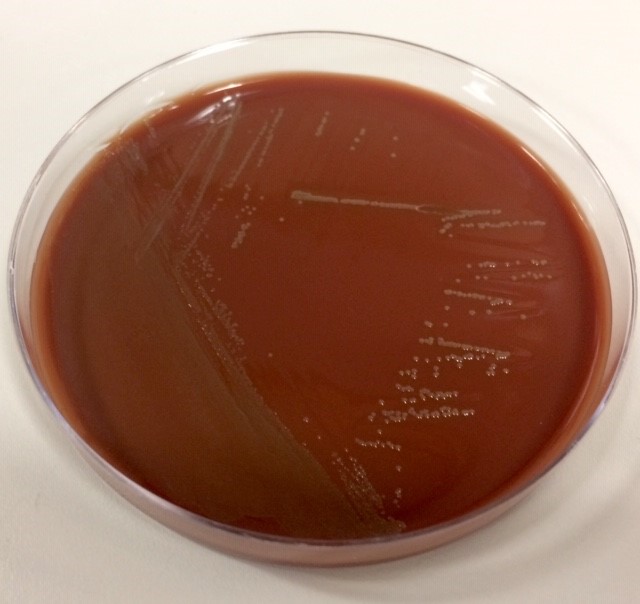
Gram stain of the blood culture bottle showed small, faintly staining gram negative, curved rods (Image 1). The patient was started on ciprofloxacin and referred to the infectious disease clinic. After 3 days of incubation, small slightly mucoid yellow gray colonies grew on 5% sheep blood and chocolate agar (Image 2). There was no growth on the MacConkey agar. Initial Gram stain revealed similar gram negative rods to the Gram stain performed on the blood culture media. MALDI-TOF identified the organism as Campylobacter jejuni. The patient was asked to stop taking ciprofloxacin and start azithromycin. She also had her port removed on this day. Four days after her oncology visit, the patient’s blood was negative for organisms. Her fever and rigors resolved as well. Susceptibility testing showed the organism to be resistant to ciprofloxacin and susceptible to azithromycin.
Discussion
Campylobacter jejuni is a small, gram negative, curved rod. It is the most common cause of bacteria-mediated diarrheal disease globally (1). In immunocompromised patients, it can cause a variety of extraintestinal diseases: septicemia, meningitis, septic arthritis, and endocarditis (2). Infection can also lead to Guillain-Barre syndrome. This is an autoimmune disease of the peripheral nerves that is thought to be due to antigenic cross reactivity between the surface lipopolysaccharides of the bacteria and the patient’s peripheral nerve gangliosides (3). Of patients diagnosed with Guillain-Barre syndrome, 20-40% will have had a history of Campylobacter jejuni infection (2).
Campylobacter jejuni grows best at 42°C in a microaerophilic environment (5% O2,10% CO2, and 80% N2). It displays a darting motility in broth and will not grow in 3.5% NaCl. Almost all are oxidase and catalase positive. On Campy-BA, a selective blood agar plate for Campylobacter jejuni, colonies will be peach colored. This media is made up of a Brucella agar base, sheep red blood cells, and various antibiotics that suppress the growth of normal fecal flora(2).
Macrolides (erythromycin, azithromycin) are considered the treatment of choice, however it has been reported that resistance approaches 1.7% (1 and 2). Fluoroquinolones like ciprofloxacin can be used, however resistance is higher due to widespread use of this drug in medical and veterinarian practices and agricultural businesses.
References
- Yang W, Zhang M, Zhou J, Pang L, Wang G, Hou F. The Molecular Mechanisms of Ciprofloxacin Resistance in Clinical Campylobacter jejuni and Their Genotyping Characteristics in Beijing, China. Foodborne Pathog Dis. 2017;14(7):386-392.
- Tille P. Bailey & Scott’s Diagnostic Microbiology. Fourteenth Edition. Elsevier;2017.
- Murray P. Medical Microbiology. Seventh Edition. Elsevier; 2013.
-Angela Theiss, MD is a 3rd year anatomic and clinical pathology resident at the University of Vermont Medical Center.

-Christi Wojewoda, MD, is the Director of Clinical Microbiology at the University of Vermont Medical Center and an Associate Professor at the University of Vermont.
