Hi everyone! It has felt so good to find myself back in the throes of hospital life. My time in the classroom during the first half of medical school was great—but this new chapter is what makes medical school very worth it. As with any new hospital, orientation was pretty run-of-the-mill: administrative paperwork, employee/student health clearance, and yet another Mantoux PPD (despite having a current QuantiFERON—lab family, you get me).
However, after all the introductory logistics, I finally reported to my first rotation. It is an elective clerkship in primary care focused primarily on patients with HIV and/or Hepatitis. My familiarity with hospital life made the transition back easy enough as I made my way to the nurses’ station looking for my attending. Being forwarded in the direction I had to go, I knocked on the door and started to introduce myself—but was abruptly interrupted. There were already two fellow student colleagues in that room with my attending and a patient. I was enthusiastically included in the process right away, and it has been non-stop since then. I am told this is a “different” rotation where I’m going to feel lucky to have so much hands-on experience, and so far, I agree. While I reminisce on these past few weeks, it’s not a specific patient or case that has stuck with me, but an overall theme I’ve noticed in this rotation. With heavy utilization of the right test at the right time (I’m sure we’re all familiar with ASCP’s Choosing Wisely campaign) and proper interpretations of lab data, patients’ chronic illnesses are being managed well and even cured.
Essentially, pharmaceuticals have been advancing so well in the last 5-10 years that treatment regimens for chronic diseases like HIV and HCV are now being actively controlled and cured, respectively. Why does this pique my interest enough to share it with all of you? As I try my best each month to provide you a window into the life of a medical lab scientist/medical student, I do so while focusing on the lab details that seem to be present in every aspect of my journey. The cures and treatments I’m currently working with are tied to lab tests like CD4 counts, viral loads, liver and kidney function tests, and many other routine values. Diagnostic criteria for different patients’ stages of hepatic damage are classified using a Child-Pugh (CTP) score from clinical information such as ascites and encephalopathy along with lab data like INR, bilirubin, and albumin. Patients with chronic conditions come back for follow up week in and week out for lab tests that let us as care providers adjust therapy accordingly. The clinic I currently rotate in provides its patients with the most up to date treatment protocols based on current literature. For example, The American Association for the Study of Liver Diseases (AASLD) and the Infectious Diseases Society of America (IDSA) regularly publish their recommendations for patients with Hepatitis C. It’s heavy reading, and anyone who goes through literature on standards of care knows it’s dense, so I’ll leave the link to the most recent guidelines on HCV testing, management, and treatment here (https://www.hcvguidelines.org/sites/default/files/full-guidance-pdf/HCVGuidance_September_21_2017_g.pdf). Actively and accurately incorporating these treatment protocols into the patient care algorithms works and demonstrates great utilization of lab driven data with new available therapies.

As a baseline it is critical to understand that patients with positive HCV antibodies will always test positive; once exposed at any point patients will remain positive. While 20% of patients can clear the infection on their own, the remaining majority develop a chronic HCV infection. There is no vaccine for HCV currently; however, there is potential to cure patients—assuming the lab values are interpreted correctly. So, we’ve established that positive HCV antibodies don’t necessarily provide diagnostic data, so the next logical step is to examine a patient’s HCV viral load. Since 2015, the New York State Department of Health established a mandate and protocol for reflex testing HCV Ab positive patients with HCV RNA viral loads. Read the public letter here (https://www.health.ny.gov/diseases/communicable/hepatitis/hepatitis_c/docs/reflex_testing_letter.pdf). While it makes logical sense, it’s still taking some time to get off the ground as I have seen patient records of different clinics’ providers ordering repeat HCV Ab testing for in-house confirmation—not the best use of resources or lab data. A clear example here of Choosing Wisely for the appropriate lab test. However, so long as HCV viral load stays undetectable by a validated testing method, patients with chronic HCV are promoted to a status of “cured HCV” and need no further testing or follow-up unless new clinical reasons appear to add testing as needed.

Protocols for treatment are based on things like genotype, cirrhosis, and naïve vs. previously failed treatment; treatment schedules last from 8 weeks up to 24 weeks. So, what does a patient’s first visit for HCV treatment therapy look like? Right away (assuming a positive HCV Ab has been obtained) a Hepatitis C RNA viral load is ordered, along with genotype (older treatments are dependent on genotype due to potential for resistance, while newer treatments are pangenotypic), hepatic fibrosis scans (because cirrhosis status determines length of treatment), PT/INR, CBC, CMP, HIV, RPR/CG and other STI screening, and urine drug testing. New generation therapies allow us to proceed despite any comorbid conditions, while maintaining upwards of 95% or greater cure rates. Coinfected patients with HIV or otherwise compromised immune systems are no longer contraindicated to receive HCV treatment. The only significant contraindication in the standards of care currently is that patients not be terminal (i.e. they must have a general prognosis of greater than 6 months).
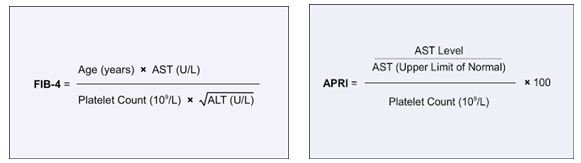
Being able to watch these treatment protocols in action is great, but one patient in particular will stay with me beyond this clerkship. We received lab results back for a male in his 60s. It was his final HCV viral load based on his treatment schedule. His chart had a box at the end of his schedule labeled “test for cure” and it had remained non-detectable the whole time through treatment. The staff at this clinic does painstaking follow-up with their patients via telephone with impressive results in patient adherence and treatment success. My task one day was to call this patient and inform him that, unless he needed any medical treatment outside of his annual physical, he no longer needed to come in for therapy or testing—his Hep C was cured. He was extremely delighted to hear this news, and I was happy to give it to him. He had been on therapy for less than a few months but had lived with HCV for years. It was an excellent experience! And even more excellent—being part of the connection between lab tests, clinics, and patients. When I started I was just excited to wear that white coat and go visit the hospital’s lab, but I was pleasantly surprised to see the impact on patients’ treatments. Especially considering using the right test at the right time, and truly making a visible difference with excellent data.
See you next time!

Post script: listen to a new podcast my colleagues and I are in where we discuss clinical stories and pearls of wisdom through medical school. As they relate to my posts here on Lablogatory I’ll include a link—this post will focus more in depth on what I presented here regarding HCV cures and lab data.

–Constantine E. Kanakis MSc, MLS (ASCP)CM graduated from Loyola University Chicago with a BS in Molecular Biology and Bioethics and then Rush University with an MS in Medical Laboratory Science. He is currently a medical student at the American University of the Caribbean and actively involved with local public health.
