Case presentation
A 79 year old female with a past medical history of COPD, hypertension, diabetes, and eczema presented to the emergency department with a localized rash on the right knee (Figure 1). The rash began after gardening and persisted for three weeks.
The patient reported some itching, warmth, and tenderness but denied nausea, vomiting, fever, and diarrhea. Her vital signs were BP 175/76| Pulse 91 | Temp 98.5 °F (36.9 °C) (Oral) | Resp 20 | SpO2 96%. The remainder of her physical exam was notable: right knee skin rash. There was no induration or fluctuance or drainage. She exhibited a full range of knee motion; there was no palpable knee joint effusion (Figure 1).

Lab CBC results were unremarkable. X-Ray knee AP and lateral – right showed soft tissue prominence anterior to the patella, which suggests prepatellar edema and a fluid collection. Lyme antibody screening was negative. Two sets of blood culture bottles were sent to the microbiology laboratory. After 24 hours of incubation, aerobic bottles were positive with the organism shown in: Gram stain (Figure 2), culture growth showing alpha-hemolytic colonies (Figure 3), H2S production on the TSA agar slant (Figure 4).
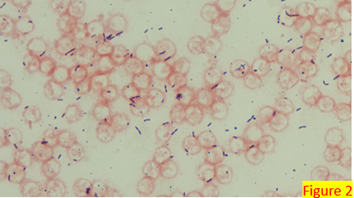
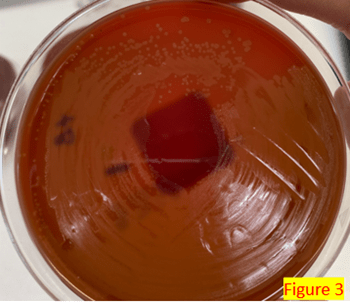

Identification by Matrix-assisted laser desorption ionization Time of flight (MALDI-ToF) revealed Erysipelothrix rusiopathiae at a score above 2.0.
Discussion
Erysipelothrix is a non-spore-forming, catalase-negative, facultative gram positive bacillus. It is not acid-fast or motile. It is distributed worldwide and is primarily considered an animal pathogen responsible for causing erysipelas that may affect a wide range of animals. Erysipelothrix is ubiquitous in soil, food scraps, and water contaminated by infected animals.1 It can survive in the soil for several weeks. In pig feces, the survival period of this bacterium ranges from 1 to 5 months.
Erysipelothrix can also cause zoonotic infections in humans, called erysipeloid. Most human infections are acquired through occupational exposure, such as fish handlers, veterinarians, and butchers, via direct injection of the organism through abrasion or injuries. Notably, the human disease of “erysipelas” is not caused by Erysipelothrix but by Streptococcus.
Erysipeloid typically develops at the site of infection between 2 and 7 days after exposure. E. rusiopathiae infection can be categorized as 1) localized cutaneous erythematous 2) generalized cutaneous form due to traumatic injury and skin penetration of the organism, and 3) septicemic form.2 Skin infection can sometimes progress to bacteremia, most commonly associated with endocarditis3. The implication of endocarditis in the setting of E. rusipathiae infection is associated with increased mortality rate.2,3
E. rusiopathiae can easily be grown on routine media, including blood and chocolate agar plates, in a clinical microbiology laboratory.1 The colonies appear as small alpha-hemolytic and can resemble alpha Streptococcus species. It can also be confused with Corynebacterium species due to the similarity in Gram stain characteristics. E. rusipathiae produces H2S on the triple iron sugar media (Figure 4), which is one of the distinguishing morphologies from other Gram-positive rods, such as Listeria or Bacillus species.1 It can be identified by Matrix-assisted laser desorption ionization Time of Flight (MALDI-ToF) directly from the positive blood culture broth (using Sepsityper Kit with Bruker MALDI-Biotyper (MBT)) or from isolated colonies.
E. rusiopathiae is generally sensitive to penicillin. It is intrinsically resistant to vancomycin and aminoglycosides.4 CLSI (Clinical Laboratory of Standard Institution) M45 ED3 recommended ampicillin or penicillin for primary testing agents.4 While antimicrobial susceptibility testing is not warranted for every case of E. rusiopathiae, it is imperative that the organism be identified due to the critical nature of infection resulting in endocarditis. Since vancomycin is typically used for broad-spectrum coverage of gram positive organisms,4 early identification of this organism and notification of clinicians is helpful for appropriate antimicrobial management.
References
- Jorgensen et.al., Chapter 27. Manual of Clinical Microbiology. 11th Edition.
2. Principe L, Bracco S, Mauri C, Tonolo S, Pini B, Luzzaro F. Erysipelothrix Rhusiopathiae Bacteremia without Endocarditis: Rapid Identification from Positive Blood Culture by MALDI-TOF Mass Spectrometry. A Case Report and Literature Review. Infect Dis Rep. 2016 Mar 21;8(1):6368. doi: 10.4081/idr.2016.6368. PMID: 27103974; PMCID: PMC4815943.
3. Wang T, Khan D, Mobarakai N. Erysipelothrix rhusiopathiae endocarditis. IDCases. 2020 Sep 9;22:e00958. doi: 10.1016/j.idcr.2020.e00958. PMID: 32995274; PMCID: PMC7508995.
4. CLSI. Methods for Antimicrobial Dilution and Disk Susceptibility Testing of Infrequently Isolated or Fastidious Bacteria. 3rd ed. CLSI guideline M45. Wayne, PA: Clinical and Laboratory Standards Institute; 2016.
-Azal Al-Ani, MD is a third-year AP/CP pathology resident at Montefiore Medical Center, Bronx, NY. She completed her medical school at Al-Anbar Medical College, Iraq. Her interest includes hematopathology and dermatopathology

-Phyu M. Thwe, PhD, D(ABMM), MLS(ASCP)CM is Associate Director of Infectious disease testing laboratory at Montefiore Medical Center, Bronx, NY. She completed her CPEP microbiology fellowship at the University of Texas Medical Branch in Galveston, TX. Her interest includes appropriate test utilization and extra-pulmonary tuberculosis.
