Hello again everyone and welcome back! Pardon the absolutely cheesy title, but this month I’d like to share parts of a clinical case and discuss some pretty important topics in pathology practice in 2021. While last month’s brief primer on the Cures Act is a definite part of the future of medicine, there are a lot of things developing in our profession—and we should all keep up!
*** Disclaimer: Please note that if/when I share cases or clinical content, they are not current, already signed out, completed and done in compliance full patient privacy guidelines. Always. ***
So let’s dive right in. A rather young male patient was sent to us from an outside facility for mildly painful, uncomfortable bilateral breast lumps. He was noted to have bilateral gynecomastia clinically and was to be evaluated via mammogram and localized needle biopsy. An ultrasound guided core needle biopsy of the left breast was collected from a mass identified on mammography.
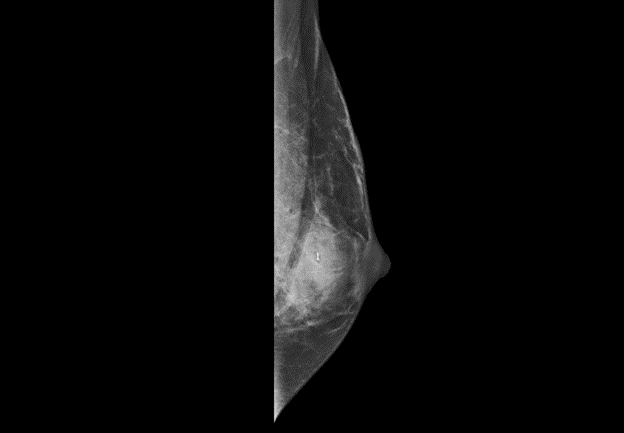
Most commonly, when evaluating gynecomastia in a male and considering the diagnostic algorithms including malignancy one worries most about ductal carcinoma: invasive, unspecified type and ductal carcinoma in situ (DCIS) pretty much round off the differential for male breast cancer. Important rule outs include clinical, hormone-related gynecomastia or otherwise relating to germ-line or chromosomal abnormalities (i.e. XXY in Klinefelter), myofibroblastoma, or unrelated distant metastases. So without too much clinical information or history—since this was an outside referral—the differential of potential considerations was pretty short therein.
The biopsy was completed shortly after mammography and was signed out as: fibroadenoma.
Wait. What?
Fibroadenomas are benign and, along with potentially malignant phyllodes tumors, come from mammary tissue, demonstrate biphasic cellular components of benign epithelium (or low-grade stroma).
Translation: to have one of these entities you need mammary tissue, specifically terminal ductal/lobular units to form the necessary architecture changes.
Simpler translation: fibroadenomas need breast tissue to be fibroadenomas.
Okay, there definitely appears to be breast tissue here to form this entity, however, it is incredibly rare for a male patient (outside of the previously mentioned conditions) to have anatomically functional lobular units. With the other etiologies ruled out, further investigation into the patient’s history was warranted. It was discovered that this patient, although male by indication on referring paperwork, actually identified as female and was on gender affirming hormone therapy for several years. A considerably simple explanation for the confounding biopsy result.
Transgender medicine and transgender pathology considerations have been talked about more in recent years than ever before. While these patients have always existed, societal changes in the last decade alone have brought to light many disparities in medical care and practice habits overall. Here on Lablogatory, there have been between 20-30 mentions of transgender patients since 2018 with entire pieces dedicated to transgender endocrinology, clinical chemistry, etc. Specific examples have included the complicated intersection of transgender care and electronic medical records, various lab values in trans patients, and an excellent overview of laboratory medicine and trans patients by Dr. Jeff SoRelle. There he discusses approaches, literature, and—most importantly—the purposeful vocabulary of transgender medicine as an empowering and informative practice.

Image 2. A 2016 paper in Laboratory Medicine highlights this patient population’s challenges to quality and equity in healthcare and establishes that gatekeepers to data—including us—should consider new ways to create inclusive laboratory medicine practices to maintain our high standard of care. Read it here.
While, this case was rather straightforward after the discovery of the patient’s history of gender affirming therapy, there are still several critical points to highlight here. First, it’s critically important in the setting of medical care to correctly and compassionately include gender identity in patient records—within the caveat of appropriate confidentiality and patient autonomy. Patient care, health management, and diagnostic efforts like ours may rely on a simple biological indication of how this patient presents and experiences their identity with relation to their clinical course. This further strengthens relationships between trans patients and their primary care providers, as well as non-patient-facing specialists like us who often put pieces of the puzzle together without an entire history at our disposal. How does this impact patient care? Simple: a trans male patient may always carry a residual indolent risk of breast cancer, while a trans female patient may need to be included in future mammogram screening. The bottom line should consider treating who you have, and screening with what you have to. Since this patient was sent because of breast lumps, as a male patient a biopsy report of “fibroadenoma” would be exceedingly rare and confounding because of normal physiology outside of specific genetic conditions. But with the right information at the right time, better patient-centered care is possible.
Finally, as a note about proper terminology, vocabulary, and available guidelines in the literature, there is both a paucity of effective transgender medical guidelines as well as a poor grasp on the terminology. Dr. SoRelle does a fantastic job with a short vocabulary outline, but we should all do better. The experiences of our trans patients is challenging to say the least, so as we continue to become stronger and closer advocates for patients in pathology and laboratory medicine, we must become familiar with their experience and advocate for the progress of inclusive medical care.
Trans patients are special, and we are specialists.
Making sure they received the highest level of care alongside all our other patients should be guaranteed. Whether in our clinical chemistry labs or surgical pathology sign outs, we already know how to create an environment of accuracy and enduring inclusion for all our patients—let’s keep it going!
Thank you for reading, I’ll see you next time!

–Constantine E. Kanakis MD, MSc, MLS(ASCP)CM is a first-year resident physician in the Pathology and Laboratory Medicine Department at Loyola University Medical Center in Chicago with interests in hematopathology, transfusion medicine, bioethics, public health, and graphic medicine. He is a certified CAP inspector, holds an ASCP LMU certificate, and xxx. He was named on the 2017 ASCP Forty Under 40 list, The Pathologist magazine’s 2020 Power List and serves on ASCP’s Commission for Continuing Professional Development, Social Media Committee, and Patient Champions Advisory Board. He was featured in several online forums during the peak of the COVID pandemic discussing laboratory-related testing considerations, delivered a TEDx talk called “Unrecognizable Medicine,” and sits on the Auxiliary Board of the American Red Cross in Illinois. Dr. Kanakis is active on social media; follow him at @CEKanakisMD.
