A 59 year old female initially presented with DCIS, treated by mastectomy and 5 years of adjuvant tamoxifen at another institution. 4 years later, she presented to another hospital with an adrenal mass, uterine fibroids, and an ovarian cyst, where a biopsy and right-sided adrenalectomy confirmed a 10.5 centimeter adrenocortical neoplasm. Margins were close, but negative at <0.1 cm. Microscopically there were areas of necrosis, high nuclear grade, a diffuse growth pattern, and clear cells representing less than 25% of the tumor. A malignancy was favored, but lack of metastasis could not confirm the diagnosis. She presented to the cancer center with stage II adrenal cancer, T2N0M0 and mitotane-induced adrenal insufficiency. Multiple hepatic and pulmonary metastases were subsequently identified and treated with extensive surgery, including a VATS wedge resection, right nephrectomy, hepatic mobilization, lysis of adhesions, dissection of the adrenal vein and vena cava with repair, and resection of an ileal mass.
Palliative radiation therapy targeted the remaining lung nodules, and six cycles of chemotherapy were administered. A CT scan-guided fine need aspiration biopsy was obtained of a 4 centimeter retroperitoneal mass that was suspicious for recurrence on imaging, which cytopathology then confirmed. Taking into consideration the history, my additional differentials included renal cell carcinoma, hepatocellular carcinoma, and plasmacytoma, with metastatic breast cancer as the least likely differential.
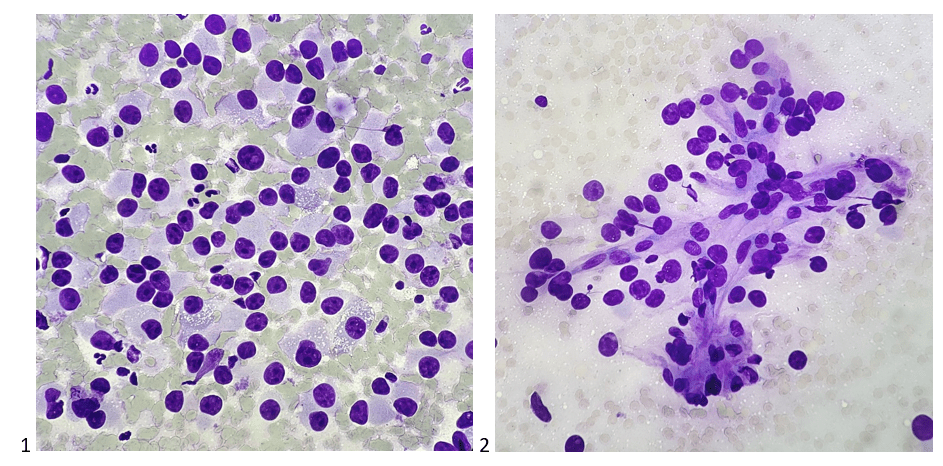
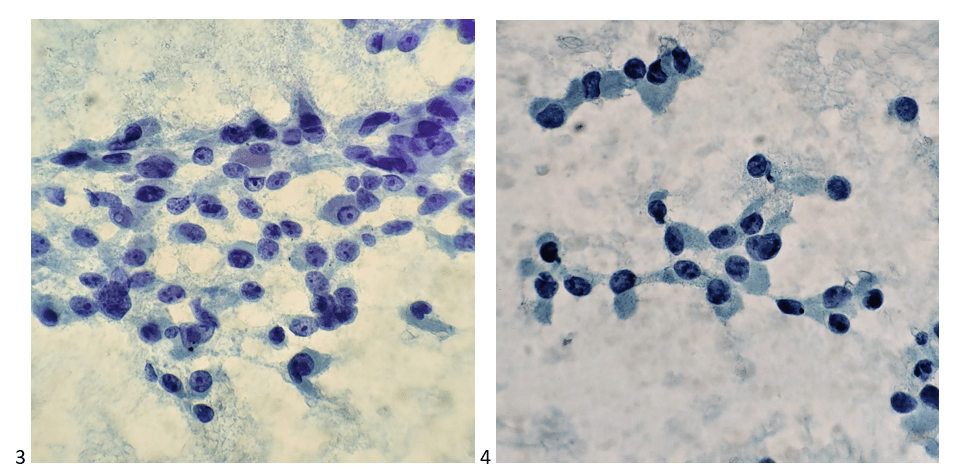

Palliative radiation therapy was then administered to the retroperitoneal and psoas masses, and microwave ablation targeted the segment 3 and segment 6 liver lesions, reducing pain and stabilizing growth, respectively. However, disease continued to slowly progress, so the oncology team sent the retroperitoneal metastasis tissue for molecular testing to assess for potential next lines of therapy. Testing revealed a variant of undetermined significance in MSH6, indeterminate tumor mutational burden, stable MSI, and negative for PDL1. When the case was brought to tumor board, the team recommended ongoing surveillance and palliative therapy (when needed) given the patient’s slowly progressing disease. Often thought of as a rare disease, I’ve examined a fair share of primary and metastatic adrenocortical carcinomas through working at a cancer center. These tiny triangular glands that sit on top of the kidneys have SO much power. Producing and regulating cortisol, aldosterone, and androgenic hormones, the adrenal cortex is an active outer layer. Whether hormonal or neoplastic, it truly is fascinating how a tiny gland could wreak so much large-scale havoc on the human body.

-Taryn Waraksa, MS, SCT(ASCP)CM, CT(IAC), has worked as a cytotechnologist at Fox Chase Cancer Center, in Philadelphia, Pennsylvania, since earning her master’s degree from Thomas Jefferson University in 2014. She is an ASCP board-certified Specialist in Cytotechnology with an additional certification by the International Academy of Cytology (IAC). She is also a 2020 ASCP 40 Under Forty Honoree.

GOOD CASE!!