One of the most effective public health strategies to date is the development of the pap smear test and its use as a screening tool in cervical cancer prevention. Before the emergence of the pap test, cervical cancer used to be the leading cause of cancer-related deaths for women in the United States.1 However, with effective pap tests screening programs and the availability of the HPV vaccine against high-risk serotypes known to be a major cause of cervical cancer, many developed countries have been able to address this disease with its attendant catastrophic consequences including loss of lives, income and long-term disabilities.
Now, cervical cancer doesn’t even make it as one of the top 10 causes of cancer-related deaths for women in the United States.2 Unfortunately, the progress that has been made with this disease is not a universal one. While many developed countries have made giant strides in addressing this disease burden, most developing countries still grapple with significant morbidities and mortalities attributable to cervical cancer. Recent statistics show that cervical cancer is the second most commonly diagnosed cancer after breast cancer and the third leading cause of cancer death after breast and lung cancers in developing countries.3 In fact, almost 90% of cervical deaths in the world occur in developing countries, with India alone accounting for 25% of the total cases.3 Cervical cancer incidence and mortality rates are highest in sub-Saharan Africa, Central and South America, South-eastern Asia, and Central and Eastern Europe.3 A combination of factors may be responsible for these discrepant findings in developing countries.
First is the lack of effective screening programs that detect precancerous lesions before they become invasive diseases. Unfortunately, this factor is linked to lack of awareness through education and sub-optimal laboratory services that still exists in many of these countries. Laboratory services are scarce and there has been a gradual decline in laboratory professionals. Even if the supplies and equipment needed to run a lab were available, where are the laboratory professionals and pathologists that are needed to provide this critical healthcare service? In addition, a lack of regulatory oversight in some of these countries makes the replication and standardization of results increasingly challenging.
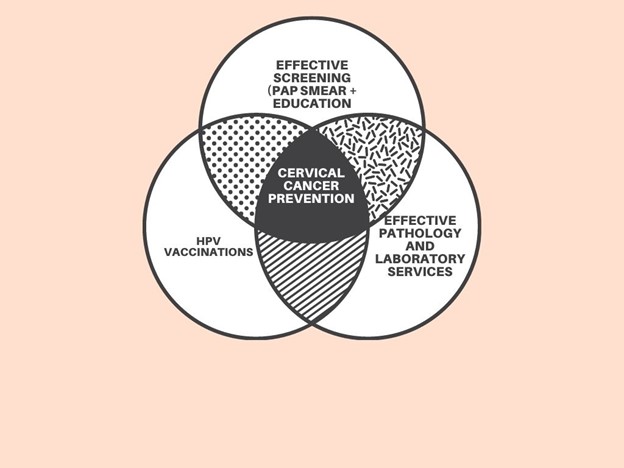
Secondly, is the role of HPV vaccinations in preventing cervical cancer. Many of these developing countries are yet to incorporate routine HPV vaccinations into their vaccination programs and access to these services are still very low. In contrast, many developed countries have made HPV vaccinations available and accessible, which is a major defense against cervical cancer.
Thirdly, is the impact of government policies on laboratory medicine. Pathology and laboratory medicine continue to face cuts in services and compensations, even in developed countries including the United States. These practices impact the ability of laboratory services to deliver optimal results, a scenario that could be even more problematic in developing nations.
As January marks cervical cancer awareness month, public health and policy professionals need to take steps to address the root causes of this problem, in order to proffer sustainable solutions, especially in developing countries. In addition to prioritizing health education and public health campaigns on cervical cancer prevention, the role of effective laboratory services in addressing these challenges also need to be emphasized.
A successful healthcare initiative requires a strong and functioning laboratory system, especially in the 21st century. Any health policy program or public health campaign that fails to recognize this fact is most likely headed for failure before it even starts off.
References
- https://www.cdc.gov/cancer/cervical/statistics/index.htm
- https://www.cancer.org/research/cancer-facts-statistics/all-cancer-facts-figures/cancer-facts-figures-2020.html
- Ferlay J, Soerjomataram I, Ervik M, Dikshit R, Eser S, Mathers C, Rebelo M, Parkin DM, Forman D, Bray F. GLOBOCAN 2012 v1.0, Cancer Incidence and Mortality Worldwide: IARC CancerBase No. 11 [Internet]. Lyon, France: International Agency for Research on Cancer. Available from: http://globocan.iarc.fr, 2013.

-Evi Abada, MD, MS is a Resident Physician in anatomic and clinical pathology at the Wayne State University School of Medicine/Detroit Medical Center in Michigan. She earned her Masters of Science in International Health Policy and Management from Brandeis University in Massachusetts, and is a global health advocate. Dr. Abada has been appointed to serve on the ASCP’s Resident’s Council and was named one of ASCP’S 40 under Forty honorees for the year 2020. You can follow her on twitter @EviAbadaMD.
