I’ve always been fascinated with medicine and the human body, knowing that I wanted to make a career of it since childhood. I was taking an elective summer course in Histology when a close relative was diagnosed with breast cancer over a decade ago, and that’s when I recognized pathology/laboratory medicine was my specialty. My questions began when her sentinel lymph node had both a different morphological picture and immunohistochemical signature than the primary tumor, and I wanted to know why. Why did her initial core biopsy only show ductal carcinoma, yet post-lumpectomy, her sentinel node was diagnosed as metastatic lobular carcinoma? Where was the second primary tumor? I needed answers, my family needed answers, and that quest propelled me to apply to Jefferson’s Master of Science in Cytotechnology program, fueling my career in Cytotechnology.
A year after I started my career at Fox Chase Cancer Center, my relative received a call – her mammogram showed two abnormal areas. Eight years after her first lumpectomy and completion of a chemotherapy and radiation regimen… eight years in remission, we both knew what this meant. I drove her to the physician’s office, and her surgeon called me into the room after he procured the core biopsies of both lesions. I saw the white “worms” of tissue in the formalin containers and felt confident of a successful procedure. I looked up to see the image of the localization wires within the tumors and heard him say, “if this does come back as cancer, which I’m fairly certain it will, we can either proceed with another lumpectomy or mastectomy.” My relative was silent the entire ride home; she needed time to process. After the not-so-surprising path report came back as ductal carcinoma in both lesions, I called her from work and said, “you’re coming to Fox Chase for a second opinion. You’re having a double mastectomy. We are NOT messing around. Not everyone gets a second chance, and I’ve seen what this care team is capable of – they know your cancer better than anyone.” She calls me her “tough cookie” both out of affection and annoyance. Little did she know my tough cookie exterior was shielding a crumbling interior. After much hesitation due to her fear of the unknown, she scheduled her second opinion.
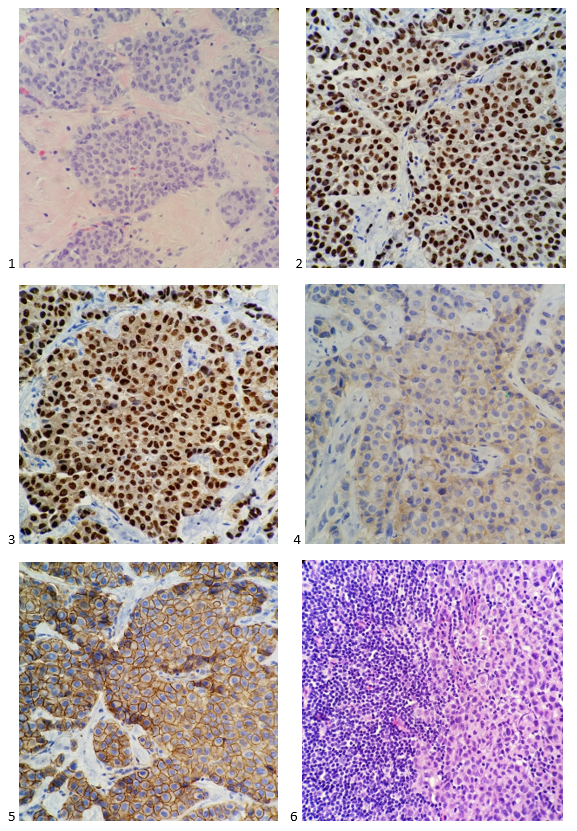
In the meantime, she had an MRI which demonstrated the two known lesions in the right breast, but also a large “enhancement” in the right breast. The MRI identified an area of enhancement in the left breast as well. And with those results, my relative felt comfortable withdrawing the lumpectomy plan from the table and played the card of double mastectomy with possible right-sided axillary lymph node dissection. A diagnosis of grade II invasive ductal carcinoma was made in the 1.5 cm right breast lesions, and the 6 cm right breast mass was diagnosed as invasive lobular carcinoma. The right axillary sentinel node demonstrated micrometastasis. On the left side, the pathology revealed a 3.5 cm grade II residual in-situ and invasive lobular carcinoma. She had a TRAM flap reconstruction at the time of her double mastectomy with radiation to the right breast after she recovered. She is tolerating and responding well to the daily dose of her aromatase inhibitor and now knows far too much about breast cancer and hormone receptor status thanks to my harping on the subject.
We both went through clinical genetics screenings, and despite our strong family history of breast cancer, no known germline mutations or variants of undetermined significance were detected in either of our peripheral blood samples. I’m already on board with the “increased lifetime risk of breast cancer” screening guidelines, and if so much as atypical ductal hyperplasia is diagnosed, I am more than willing to have a semi-prophylactic double mastectomy, just to reduce my overall risk of both carcinoma AND recurrence. My relative’s breast cancer experience set the precedence for my approach in the field of cytotechnology. From the beginning, I craved definitive answers for her, and I will do whatever I can as a cytotechnologist to provide definitive answers for all of my patients.
I still remember attending my first ultrasound-guided FNA (Fine Needle Aspiration) after my relative’s mastectomy. The patient was 42, a mother to a 3 year old and 6 year old, and presented with triple negative, grade III, poorly differentiated breast cancer and cervical, occipital, hilar, and mediastinal lymphadenopathy.
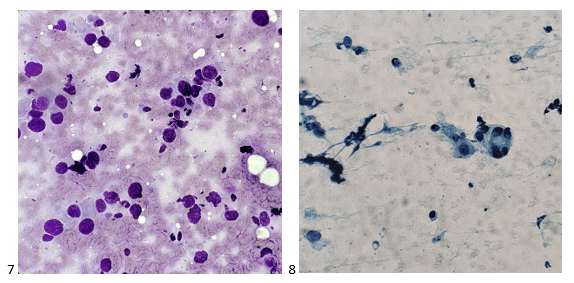
I assisted the radiologist in obtaining cellular material from the patient’s targeted right cervical lymph node, and when the radiologist prepared the core biopsy needle, the patient started to tear up, knowing well what the lymphadenopathy indicated. She told us she knows how aggressive her cancer is, how her young children are going to lose their mom, and I remember doing everything I could to hold it together and provide my adequacy statement to the radiologist. Like a child on the playground trying not to cry in front of her friends after skinning her knee, I gathered all my paperwork and the specimen containers, cleaned up my cytology cart, and walked back upstairs to our cytoprep lab. I assigned the specimen an accession number, handed the prep tech my cell block tube so she could spin down the residual material in formalin and ensure the cold ischemic time was less than one hour, and I bee-lined for a private space. I found our cytology file room, closed the door behind me, sank against the wall, and cried. I, too, knew the likelihood of her children losing their mom without medical intervention, and that the intent to cure would be the most difficult journey of this young woman’s life. This is why I’m here. This is why I fight for more material, why I fight for answers, and why I will always put the patient first.

Taryn Waraksa, MS, SCT(ASCP)CM, CT(IAC), has worked as a cytotechnologist at Fox Chase Cancer Center, in Philadelphia, Pennsylvania, since earning her master’s degree from Thomas Jefferson University in 2014. She is an ASCP board-certified Specialist in Cytotechnology with an additional certification by the International Academy of Cytology (IAC). She is also a 2020 ASCP 40 Under Forty Honoree.
