The general public doesn’t always know a lot about laboratory testing in general, but most people know a little about blood types, even if it’s what they have learned from TV! Blood types do seem to come up in casual conversation. We might hear a conversation about blood type after someone has donated blood, or between family members comparing notes, who ask “What’s your type?” Yet, even with medical technologists, there can still be some confusion about blood types and blood typing, particularly if one has not worked in Blood Bank in many years. I recently received an email from a colleague who had a few questions about blood types, as she has not worked in Blood Bank for over 40 years. I always tell my students that no question is a bad question, and indeed, she asked some very good questions, which I will address with this case study.
- What blood type is listed on a patient’s chart if they type “O Du”?
- What blood type is recorded on a donated unit of blood typed “O Du”?
- What type of blood does an “O Du” patient receive?
- Can an “O Du” patient have a transfusion reaction if they are transfused with O positive blood? Would she need to receive O negative blood in a transfusion?
- Does an “O Du” patient need to receive RhoGAM if she pregnant and her husband is Rh positive?
If you have ever wondered or can’t remember details about any of these questions, you’re in the right place. So, what’s new, if anything, with blood types?
Landsteiner discovered the ABO blood group system in 1901, and identified A, B and O blood types, using experiments performed on blood from coworkers in his laboratory. The discovery of the codominant AB blood type soon followed, but it was not until around 1940 that the Rh blood group was first described. In 1946, Coombs and coworkers described the use of the antihuman globulin (AHG) to identify weak forms of Rh antibodies in serum. For us old blood bankers, the original name for this test was the Coombs’ test. (You will still find physicians ordering a Coombs’ test!) The current and proper name for this is the direct antibody test (DAT), which is used to detect in vivo sensitization of RBCs. AHG can also be used to detect in- vitro sensitization of RBCs using the 2 stage indirect antibody test (IAT).
Since Landsteiner’s work, we have not discovered any new blood groups that are part of the routine blood type. The ABO and Rh blood groups are still the most significant in transfusion medicine, and are the only groups consistently reported. However, we currently recognize 346 RBC antigens in 36 systems.1 Serological tests determine RBC phenotypes. Yet, today we can also determine genotype with family studies or molecular testing. This case study and 2 part blog reviews some terminology in phenotyping, some difficulties and differences encountered, and explores the possibility of RHD genotyping to assess a patient’s true D status.
Our case study involves a 31 year old woman who is newly married. She is not currently pregnant, has never been pregnant, is not scheduled for surgery but has had a prior surgery 15 years ago, and has never received any blood products. She and her husband recently donated blood and, as first time blood donors, just got their American Red Cross (ARC) blood donor cards in the mail. The husband noted that his card says that he is type O pos. The woman opens her card, and, with a puzzled look on her face, says “My card says I’m an O Pos, too. There must be a mistake.” She knows she has been typed before and checks her MyChart online. Sure enough, her blood type performed at a local hospital is listed in her online MyChart as O negative. She further checks older printed records and discovers that 15 years ago, before surgery, she was typed at a different hospital as “O Du”. She is very upset, wondering how she can have 3 different blood types. She is additionally concerned because they are planning to have children and recalls being told that because she is Rh negative, that she would need Rhogam. Is she Rh negative or positive, and what does Du mean? Will she need Rhogam when pregnant? She has many questions and calls the ARC donor center for an explanation.
What blood type is listed on a patient’s chart if they type “O Du”?
What is happening here, what is this woman’s actual blood type, and what testing can be done to ensure accuracy in Rh typing? From the patient reports, it appears that this woman has what today we call a “weak D.” Du is an older terminology that should no longer be used, and that has been replaced by the term “weak D.” But, why does she have records that show her to be an O neg, a type O, Du (today, this would be written O weak D), and now, a card from ARC stating she is O pos?
RhD negative phenotypes are ones that lack detectable D antigen. The most common Rh negative phenotype results from the complete deletion of the RHD gene. Serologic testing with anti-D is usually expected to produce a strong 3+ to 4+ reaction. A patient with a negative anti-D at IS and at IAT would be Rh negative. If the patient has less than 2+ strong reaction at immediate spin (IS), but reacts at IAT, they would be said to have a serologically weak D.1 Historically, weak D red blood cells (RBCs) are defined as having decreased D antigen levels which require the IAT for detection. Today’s reagents can detect many weak D types that may have been missed in the past, without the need for IAT. However, sometimes IAT is still necessary to detect a weak D. When this is necessary is dependent on lab SOPs and whether this is donor testing or patient testing. The reported blood type of this patient also depends on the SOPs of the laboratory that does the testing. And, the terminology used for reporting is also lab dependent. It is not required by AABB to test patient samples for weak D (except for babies of a mother who is D negative). There is also no general consensus as to the terminology to be used in reporting a weak D. Some labs would result this patient as O negative, weak D pos. Some labs may result O pos, weak D pos. Others may show the individual reactions but the resulted type would be O pos. Labs who do not perform weak D testing would report this patient as O, Rh negative. The following chart explains why this patient appears to have 3 types on record.
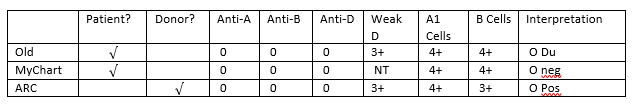
What blood type is recorded on a donated unit of blood typed “O Du?”
AABB Standards for Blood Banks and Transfusion Services requires all donor blood to be tested using a method that is designed to detect weak D. This can be met through IAT testing or another method that detects weak D. If the test is positive, the unit must be labeled Rh positive. This is an important step to prevent alloimmunization in a recipient because weak D RBCs can cause the production of anti-D in the recipient. This also explains why the ARC donor card this patient received lists her type as O pos.
What type of blood does an “O Du” patient receive?
Historically, weak D red blood cells (RBCs) were defined as having decreased D antigen levels which require the IAT for detection. A patient who is serologic weak D has the D antigen, just in fewer numbers. This type of weak D expression primarily results from single-point mutation in the RHD gene that encodes for a single amino acid change. The amino acid change causes a reduced number of D antigen sites on the RBCs. Today we know more about D antigen expression because we have the availability to genotype these weak D RBCs. More than 84 weak D types have been identified, but types 1, 2, and 3 represent more than 90% of all weak D types in people of European ethnicity.2 An Rh negative patient has no D antigen and should, under normal circumstances, only receive Rh negative blood. Yet, there has been a long history of transfusing weak D patients with Rh positive RBCs. 90% of weak D patients genotype as Type 1, 2 or 3 and may receive Rh positive transfusions because they rarely make anti-D. 2
It is now known that weak D can actually arise from several mechanisms including quantitative, as described above, position effect, and partial D antigen. Molecular testing would be needed to differentiate the types, but, with the position effect, the D antigen is complete and therefore the patient may receive Rh positive blood with no adverse effects. On the other hand, a partial D patient may type serologically as Rh negative or Rh positive and can be classified with molecular testing. It is important to note that these partial D patients are usually only discovered because they are producing anti-D. If anti-D is found, the patient should receive Rh negative blood for any future transfusions.
Thus, 3 scenarios can come from typing the same patient. With a negative antibody screen, and because 90% of weak D patients have been found to be Type 1, 2 or 3 when genotyped, many labs do not routinely genotype patients and will report the blood type as Rh pos and transfuse Rh pos products. However, depending on the lab medical director and the lab’s SOPs, these same patients may be labeled Rh neg, weak D and receive Rh negative products. There is no general consensus on the handling and testing of weak D samples. The 3rd scenario is that many labs do not test for weak D in patients at all, and a negative D typing at IS would result in reporting the patient as Rh neg, with no further testing. In this case, the patient would be transfused with Rh negative products.
Can an “O Du” patient have a transfusion reaction if they are transfused with O positive blood? Would she need to receive O negative blood in a transfusion?
This question was covered somewhat in the above discussion. Policies regarding the selection of blood for transfusion are lab dependent, dictated by the lab medical director, and are based on the patient population, risk of developing anti-D, and the availability or lack of availability of Rh negative blood products. Anti-D is very immunogenic. Less than 1 ml of Rh pos blood transfused to an Rh negative person can stimulate the production of anti-D. However, not all patients transfused with Rh positive blood will make and anti-D. As discussed above, 90% of weak D patients are types 1, 2 or 3, would be unlikely to become alloimmunized to anti-D. If a weak D patient with a negative antibody screen receives a unit of D pos RBCs, there is a very small possibility that they are a genotype who could become alloimmunized to the D antigen and produce anti-D. However, as stated above, the majority of weak D patients can be transfused with D positive RBCs. Thus, with few exceptions, from a historical perspective, one can safely classify the weak D as D positive.
This question gets a little trickier when dealing with females of childbearing age. We particularly want to avoid giving Rh positive blood to females to avoid anti-D and the complications of Hemolytic Disease of the Fetus and Newborn. Therefore, when dealing with these patients, lab policies and physicians tend to be more conservative in their approach to transfusion. The consequences, however, in males and older females are less serious and these patients could be given Rh positive blood if there exists a shortage of Rh negative units. Any patient who becomes alloimmunized to the D antigen, would thereafter be transfused with Rh negative products.
Does an “O Du” patient need to receive RhoGAM if she pregnant and her husband is Rh positive?
This, again, would be up to the medical director, the lab’s SOPs or the patient’s physician. Depending on lab practice, the lab may or may not perform weak D testing. If the lab does not perform weak D and results this patient as Rh neg, the patient would get Rhogam. If the lab does do weak D testing and finds a weak D phenotype, the decision whether or not to give Rhogam would be up to lab practices and the practitioners involved. The lab’s policy on terminology used in resulting the type may also reflect the decision whether or not to give Rhogam. This brings up a lot of questions in the lab because we know that a patient who would not make anti-D would not need Rhogam. So, what is the best course of action? Read my next blog to learn more about troubleshooting and resolving D typing discrepancies!
From the discrepancies in reported type in this individual, and putting all the pieces of the puzzle together, we can conclude that this patient is a weak D phenotype. However, the type reported and the terminology used varies from lab to lab. Molecular testing is available, yet most labs are still using serological testing for blood types for both donors and patients. This is based on several factors within the lab setting. Stay tuned for my next Blood Bank blog exploring D typing discrepancies and the financial aspects of performing genotype on pregnant patients to clarify Rh type.

-Becky Socha, MS, MLS(ASCP)CM BB CM graduated from Merrimack College in N. Andover, Massachusetts with a BS in Medical Technology and completed her MS in Clinical Laboratory Sciences at the University of Massachusetts, Lowell. She has worked as a Medical Technologist for over 30 years. She’s worked in all areas of the clinical laboratory, but has a special interest in Hematology and Blood Banking. When she’s not busy being a mad scientist, she can be found outside riding her bicycle.
