A patient with no previous cancer history presented to the Head and Neck Clinic after imaging performed for radial nerve palsy detected multiple (4) thyroid nodules. The 1.9 centimeter isthmus nodule met biopsy criteria due to its size, hypoechogenicity, solid composition, and punctate echogenic foci, placing the nodule into a TI-RADS risk category of TR5. An ultrasound-guided fine needle aspiration (FNA) was performed, and Rapid Onsite Evaluation (ROSE) determined that the sample contained atypical follicular cells. Two additional passes were collected in Veracyte Afirma fixative to be reflexed for a Gene Sequencing Classifier in the event of an indeterminate final diagnosis, such as follicular lesion of undetermined significance (FLUS), atypia of undetermined significance (AUS), or suspicious for follicular neoplasm. The Diff-Quik smears, featuring nuclear inclusions and papillary formations, are presented below.
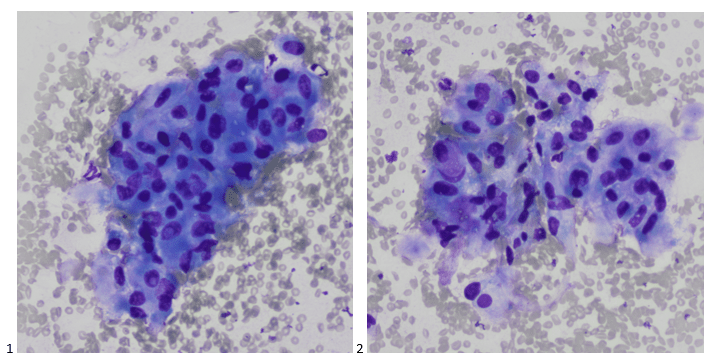
The following day, the Pap-stained smears demonstrated more pronounced cytologic features of papillary thyroid carcinoma, including nuclear invaginations, nuclear grooves, papillary clusters, and limited colloid. Rare tumor cells were also identified on cell block sections (not shown), and immunohistochemical (IHC) stains showed that the cells of interest were positive for thyroglobulin and TTF-1. Although there were a few pleomorphic and histiocytic areas on the smears which appeared different than classic papillary thyroid carcinoma, the thyroid isthmus FNA was signed out as papillary thyroid carcinoma (Bethesda Category VI), and correlation with clinical and radiological findings was recommended.
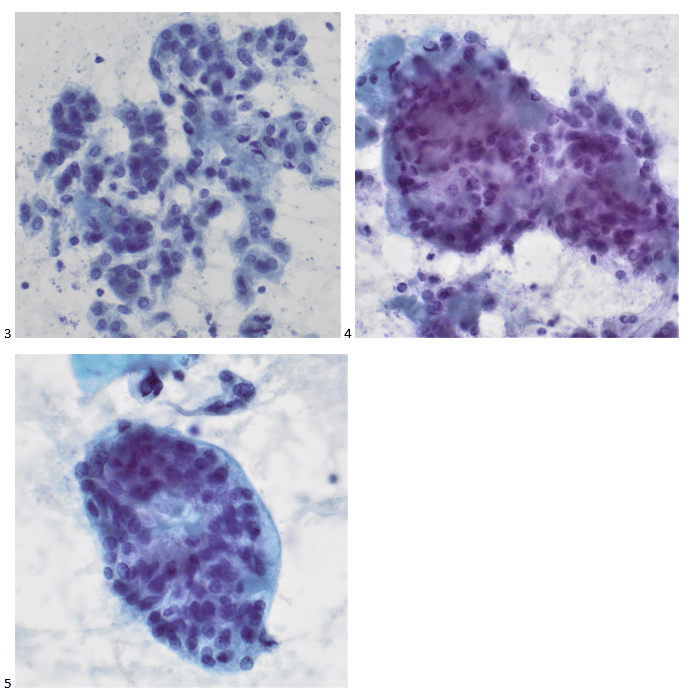
Due to the final cytology diagnosis, the patient was scheduled for a total thyroidectomy and possible neck lymph node dissection within three weeks of the initial biopsy. During the total thyroidectomy, the 2 centimeter isthmus nodule was noted, and there was no gross evidence of extrathyroidal extension or suspicious lymphadenopathy, as this was diagnosed as non-invasive follicular thyroid neoplasm with papillary like nuclear features (NIFTP). Adjacent to the NIFTP, but still within the isthmus, was a 1.6 cm hyalinizing trabecular tumor, which alludes to the other cells of interest identified on the FNA smears. No tumor was identified in three lymph nodes, and a less than 0.1 cm incidental micropapillary thyroid carcinoma (follicular variant) was found. The margins were negative for all three elements.
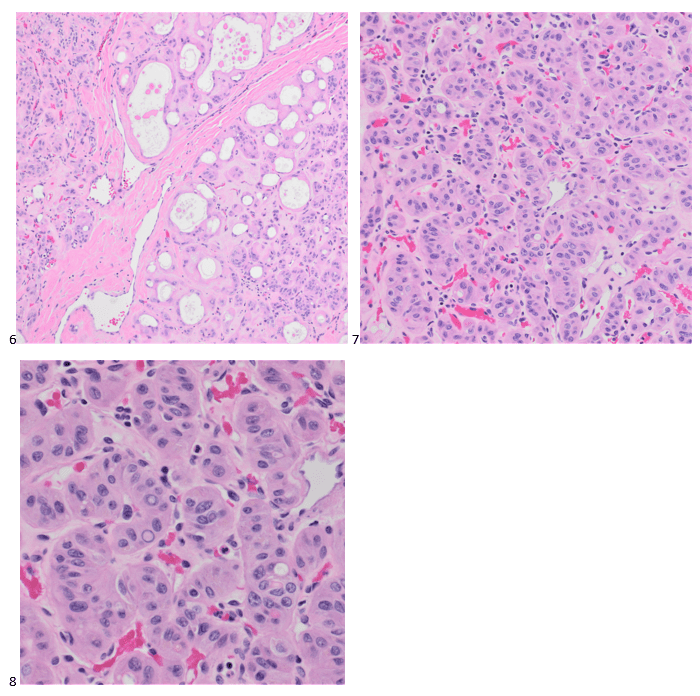
IHC was performed on the dominant isthmus nodule showing that the tumor cells are positive for TTF-1, thyroglobulin, and PAX-8, while negative for calcitonin. Ki-67/MIB1 at 37 degrees Celsius demonstrated no membranous staining, supporting the diagnosis of NIFTP. The same stains were performed on the neighboring 1.6 isthmus tumor with all of the immunostains yielding the same results, except positivity in Ki-67/MIB1. This single stain differentiates a diagnosis of hyalinizing trabecular tumor, a very rare (less than 1%) follicular-derived thyroid tumor that has strikingly similar features to papillary thyroid carcinoma and NIFTP.1 While hyalinizing trabecular tumors are typically a histologic diagnosis due to the solid trabecular growth pattern, hyalinization of extracellular spaces and lack of vascular or capsular invasion, careful cytologic analysis could postulate the presence of this tumor especially in FNAs that do not demonstrate classic papillary thyroid carcinoma features.1 It is important to note, especially in hindsight thanks to this case, that the histiocytic cells identified on the FNA smears had elongated nuclei with abundant cytoplasm and cells radially arranged around hyaline globules. While nuclear grooves and intranuclear inclusions are prominent in both tumors, the nuclear shape and presence of hyaline can help cytologists morphologically distinguish between papillary thyroid carcinoma and hyalinizing trabecular tumors and trigger the inclusion of MIB1 IHC staining (LiVolsi, 2022).
References
- LiVolsi VA. (17 May 2022). Hyalinizing trabecular tumor. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/thyroidhtn.html. Accessed May 27th, 2022.

-Taryn Waraksa-Deutsch, MS, SCT(ASCP)CM, CT(IAC), has worked as a cytotechnologist at Fox Chase Cancer Center, in Philadelphia, Pennsylvania, since earning her master’s degree from Thomas Jefferson University in 2014. She is an ASCP board-certified Specialist in Cytotechnology with an additional certification by the International Academy of Cytology (IAC). She is also a 2020 ASCP 40 Under Forty Honoree.
