Case Presentation
An adult presented to the emergency department with a finger infection persisting for the past 14 days after being bitten by her dog. The finger was swollen, tender and red but the patient denied fever, chills, or purulent drainage. The patient was previously given 10 days of doxycycline and amoxicillin-clavulanic acid without any improvement. The patient underwent incision and drainage and the specimen was sent for aerobic culture and Gram stain. No organisms or WBCs were seen on the Gram stain. On day 3 of incubation, a yellow colony was observed on the chocolate agar. The colony was streaked out onto another chocolate plate for subculture (Image 1). MALDI-TOF identified this organism as Neisseria animoralis.
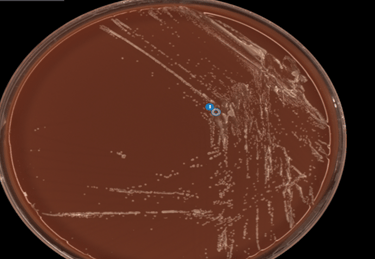
Discussion
Neisseria animoralis and Neisseria zoodegmatis are primarily zoonotic organisms found as normal oral flora of cats and dogs. Both can cause wound infections in humans following animal bites. However, these organisms are under recognized animal bite pathogens, often leading to their identifications being dismissed as contaminants. While there are limited published studies on this organism, it is important to recognize its role in wound infections, as in our case. Due to lack of awareness and reduced recovery in culture, case studies have shown correlations with this organism and poor healing and chronic wound infections.
On Gram stain, N. animoralis appears as a Gram negative coccoid rod. In culture, N. animoralis is a slow growing organism that produces yellow or white colonies that are shiny and smooth. N. animaloris produces acid from glucose, but not lactose, sucrose, or maltose. MALDI-TOF is most commonly used for identification.
Limited N. animoralis treatment data are available currently. Most animal bite-related infections are polymicrobial in nature and thus, antibiotic treatment is broad spectrum to cover the most common aerobic and anaerobic organisms.
Resources
- Johannes Elias, Matthias Frosch, and Ulrich Vogel, 2019. Neisseria, In: Carroll KC, Pfaller MA Manual of Clinical Microbiology, 12th Edition. ASM Press, Washington, DC. doi: 10.1128/9781683670438.MCM.ch36
- Heydecke A, Andersson B, Holmdahl T, Melhus A. Human wound infections caused by Neisseria animaloris and Neisseria zoodegmatis, former CDC Group EF-4a and EF-4b. Infect Ecol Epidemiol. 2013;3:10.3402/iee.v3i0.20312. Published 2013 Aug 2. doi:10.3402/iee.v3i0.20312
- Kathryn C. Helmig, Mark S. Anderson, Thomas F. Byrd, Camille Aubin-Lemay, Moheb S. Moneim, A Rare Case of Neisseria animaloris Hand Infection and Associated Nonhealing Wound, Journal of Hand Surgery Global Online, Volume 2, Issue 2, 2020, Pages 113-115, ISSN 2589-5141 https://doi.org/10.1016/j.jhsg.2020.01.003.
- Merlino J, Gray T, Beresford R, Baskar SR, Gottlieb T, Birdsall J. Wound infection caused by Neisseria zoodegmatis, a zoonotic pathogen: a case report. Access Microbiol. 2021;3(3):000196. Published 2021 Feb 10. doi:10.1099/acmi.0.000196

-Paige M.K. Larkin, PhD, D(ABMM), M(ASCP)CM is the Director of Molecular Microbiology and Associate Director of Clinical Microbiology at NorthShore University HealthSystem in Evanston, IL. Her interests include mycology, mycobacteriology, point-of-care testing, and molecular diagnostics, especially next generation sequencing.
