Case History
An adult male presented to the Emergency Department with edema and pain in his left hand. The patient stated that he was bitten by his cat 24 hours prior to admission. Bloodwork was drawn and patient was found to have mild leukocytosis (11.2 x103 cells/uL [reference range, 4-10 x103 cells/uL]) with an elevated neutrophil percentage (76.8% [reference range, 40-70%]). Debridement was performed in the operating room and purulent drainage was send to the lab for aerobic and anaerobic bacterial culture. Gram stain of the purulent drainage showed 3+ white blood cells and mixed bacteria. Mixed aerobic flora grew out in culture, but the predominate isolate was Pasteurella multocida, which grew on 5% sheep blood and Chocolate agar plates (Figure 1) as identified using MALDI-TOF MS.
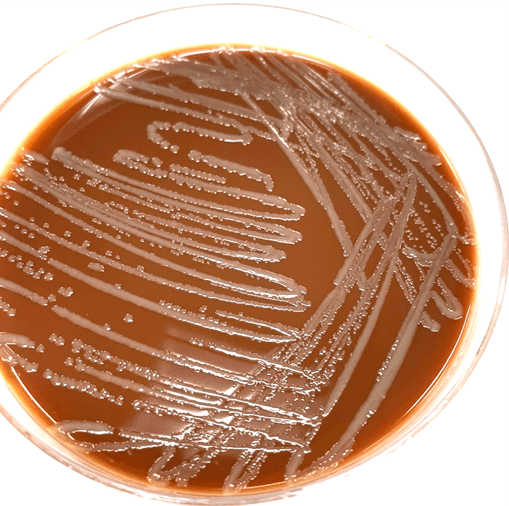

Pasteurella multocida
Pasteurella multocida is one of the most common causes of animal bite-related bacterial infections among patients who present to the Emergency Department in the United States.1 Immunocompetent patients with P. multocida infection typically present with cellulitis at the site of physical injury. These infections usually have a rapid course that can develop within 3 – 48 hours following injury. While most commonly associated with animal bites, immunocompromised patients can acquire Pasteurella simply through animal contact. These rare cases can present as more severe infections involving the respiratory tract and invasive infections including meningitis and endocarditis.
P. multocida is a small, non-motile, facultative anaerobe, which contains an outer polysaccharide capsule. The outer polysaccharide capsule is used to further classify serogroup with most human infections caused by serogroups A and D.2 Further classification into sub-serogroups is determined by the composition of the outer lipopolysaccharide (LPS), which further separates isolates into 16 serovars.3 The bacterium stains as a Gram negative coccobacillus (Figure 2). The recommended growth medium to grow Pasteurella multocida is 5% sheep’s blood agar.4 Of note, P. multocida does not grow on MacConkey agar, unlike most other Gram negative organisms, which can aid in identification of the organism. Most strains of the bacterium test positive for oxidase, catalase, and indole.2
While P. multocida is typically susceptible to penicillin,5 due to the polymicrobial nature of animal bites, broad-spectrum anaerobic and oral flora coverage is recommended for animal bite-related infections. Often, amoxicillin-clavulanate (Augmentin) is used, which will cover the most common organisms including Pasteurella species. Antibiotics which should be avoided for therapy include cephalexin, dicloxacillin, and erythromycin as they have been shown to have inadequate activity against the bacterium.6
References
- Martin TCS, Abdelmalek J, Yee B, Lavergne S, Ritter M. Pasteurella multocida line infection: a case report and review of literature. BMC Infect Dis. 2018 Aug 23;18(1):420.
- Wilson BA, Ho M. Pasteurella multocida: from zoonosis to cellular microbiology. Clin Microbiol Rev. 2013 Jul;26(3):631-55.
- Harper M, Boyce JD, Adler B. The key surface components of Pasteurella multocida: capsule and lipopolysaccharide. Curr Top Microbiol Immunol. 2012;361:39-51.
- Lariviere S, Leblanc L, Mittal KR, Martineau GP. Comparison of isolation methods for the recovery of Bordetella bronchiseptica and Pasteurella multocida from the nasal cavities of piglets. J Clin Microbiol. 1993 Feb; 31(2):364-7.
- Hasan J, Hug M. Pasteurella Multocida. [Updated 2021 May 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557629/
- Stevens DL, Bisno AL, Chambers HF, Dellinger EP, Goldstein EJ, Gorbach SL, Hirschmann JV, Kaplan SL, Montoya JG, Wade JC. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the infectious diseases society of America. Clin Infect Dis. 2014 Jul 15;59(2):147-59.

-Tristan R. Grams, is a PhD Candidate at the University of Florida in Gainesville, FL where he studies HSV-1 latency and characterizing SARS-CoV-2 antiviral agents.

-Paige M.K. Larkin, PhD, D(ABMM), M(ASCP)CM is the Director of Molecular Microbiology and Associate Director of Clinical Microbiology at NorthShore University HealthSystem in Evanston, IL. Her interests include mycology, mycobacteriology, point-of-care testing, and molecular diagnostics, especially next generation sequencing.
