Clinical History
A 30 year old African American male presented to the emergency department (ED) with fevers and cough. His past medical history was significant for type 1 diabetes & diabetic nephropathy requiring a kidney/pancreas transplant three years prior. He is compliant with his immunosuppressant regimen. He described the cough as non-productive and denied shortness of breath or chest pain. He denied sick contacts, recent travel, and has no pets. After hospital admission, he became septic, developed severe hypotension (70/30s), and was transferred to the intensive care unit (ICU). Chest x-ray showed multifocal consolidations in bilateral lung fields and a small pleural effusion consistent with pneumonia. He was empirically started on vancomycin, piperacillin-tazobactam, azithromycin, and micafungin. Infectious diseases was consulted and recommended a board variety of tests and cultures given the patient immunosuppressed status.
Laboratory Identification
The following results were obtained:
Sputum culture: normal respiratory flora, negative for fungi and acid fast bacilli
Streptococcus pneumoniae & Legionella pneumophila antigens: negative
Histoplasma & Blastomyces urinary antigens: negative
Fungitell: negative
Respiratory viral PCR panel: positive for adenovirus, coronavirus, and rhinovirus

Given this positive serum result for Cryptococcus neoformans despite multiple negative sputum cultures, a bronchoalveolar lavage & lumbar puncture were performed and bacterial & fungal cultures were performed.
Discussion
Cryptococcus neoformans is an encapsulated yeast that is most commonly acquired through inhalation and can infect & disseminate to multiple organ systems including the lungs, central nervous system, skin and bones, especially in immunocompromised patients such as those with HIV or organ transplant patients. The thick polysaccharide capsule gives colonies of C. neoformans a mucoid appearance, serves as a major virulence factor, and also plays an important part in various laboratory identification methods.
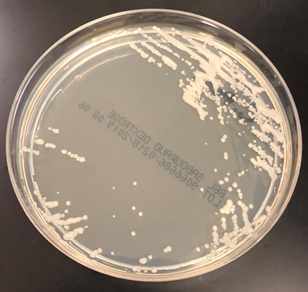
In the lab, C. neoformans will grow a variety of selective and non-selective agars including blood, chocolate, Sabouraud dextrose, and cornmeal agars as discrete, cream colored colonies (Image 2). On microscopic examination, the C. neoformans yeast are gram positive with narrow based budding and a thick capsule. The yeast vary in size from 2-20 µm and are evenly spaced from one another due to the capsule. C. neoformans is positive for both urease and phenoloxidase. Historically, India ink stain was performed on CSF specimens to highlight the capsule using direct microscopy. Grocott’s methenamine silver (GMS), mucicarmine, and Fontana-Masson histochemical stains are all positive for C. neoformans.
Cryptococcal antigen tests directed to the capsular polysaccharide can also be used to diagnosis C. neoformans infections from both serum and CSF specimens. Common methods include immunochromatographic lateral flow assays or particle agglutination. Advantages to these methods include increased sensitivity and the ability to provide semi-quantitative titer results which can be used to monitor the patient’s response to therapy. Rarely, false negative results can occur due to extremely high concentrations of the cryptococcal antigen. In order to combat the prozone effect, the sample should be diluted prior to repeating the test if there is a high suspicion of cryptococcal infection. False positive results may also occur when macroglobulins are present in the sample due to disease states such as rheumatoid arthritis or lupus. Use of pronase can prevent the interference of macroglobulins on serum test results. False positive test results have also be documented due to interferences from various collection devices such as anaerobic vials.
In the case of our patient, as C. neoformans is intrinsically resistant to echinocandins, he was switched from micafungin to fluconazole. He responded well and after completing the therapeutic course, he continued on a prophylactic dose of fluconazole. His cerebrospinal fluid culture showed no growth and the cryptococcal lateral flow assay was negative on the CSF specimen.
-Charles Middleton, MD, is a first year Anatomic and Clinical Pathology resident at the University of Mississippi Medical Center.

-Lisa Stempak, MD, is an Assistant Professor of Pathology at the University of Mississippi Medical Center in Jackson, MS. She is certified by the American Board of Pathology in Anatomic and Clinical Pathology as well as Medical Microbiology. She is the Director of Clinical Pathology as well as the Microbiology and Serology Laboratories. Her interests include infectious disease histology, process and quality improvement, and resident education.
