Case History
14 year old cystic fibrosis (CF) patient was admitted to the hospital for a CF exacerbation with a known rhinovirus infection. The patient reported congestion and cough with production of greenish sputum. The following was isolated from a sputum culture.
Laboratory Culture
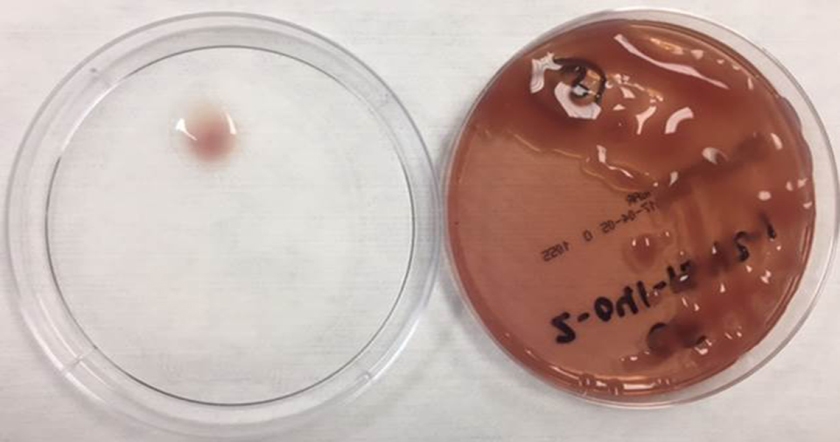
Image A. MacConkey Agar plate with mucoid Pseudomonas aeruginosa colonies.
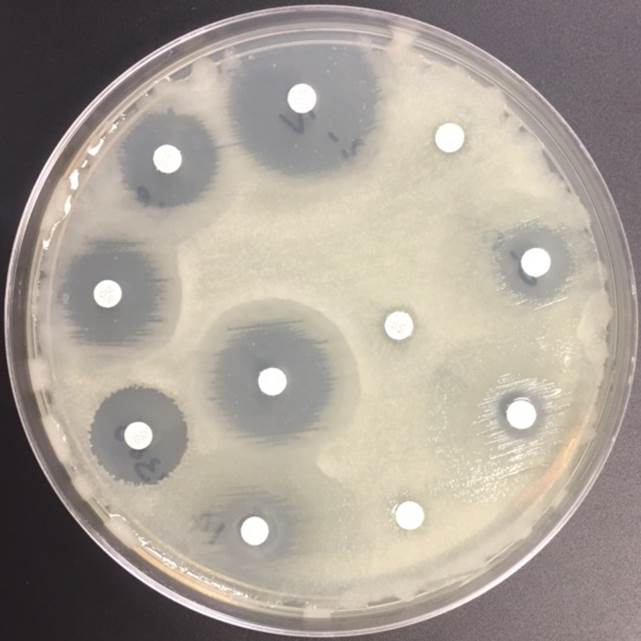
Image B. Kirby-Bauer Method of antimicrobial susceptibility.
Discussion
Cystic fibrosis patients have complex polymicrobial respiratory flora. Routine cultures may reveal different bacterial species that can contribute to the difficulty in treating and preventing infections in these patients. Staphylococcus aureus, Haemophilus influenza and Pseudomonas aeruginosa are main contributors to the infections found in CF patients.
In this case, we isolated a mucoid Pseudomonas aeruginosa (Image A). Pseudomonas aeruginosa is an oxidase-positive, gram negative rod-shaped bacterium that is commonly found in the environment. It is considered a severe and frequent pathogen in patients with cystic fibrosis. In chronic infections, it is thought that P. aeruginosa can undergo a “mucoid switch” where the bacterium can acquire mutations that lead to the mucoid phenotype. The phenotype is so impressive that excess polysaccharide will often drip onto the lid of the plate when stored upside down during incubation.
One of the key features of mucoid strains of P. aeruginosa is their ability to form biofilms. Biofilms consist of a matrix of polysaccharide, protein and DNA. This provides not only a protective barrier from antibiotics and the immune system, but also may contribute to the growth of other bacteria within the microenvironment.
With all the excess polysaccharide, it can be difficult to standardize the inoculum of mucoid isolates of P. aeruginosa which is an essential starting point for the microbroth dilution method of antimicrobial susceptibility testing. For this reason, susceptibility testing of mucoid isolates is often performed by Kirby-Bauer (KB) disk diffusion method. The KB method is a test of antimicrobial susceptibility that is based on the zone of inhibition surrounding disks that contain antimicrobial drugs (Image B). The strain of mucoid P. aeruginosa isolated in this case was found to be susceptible to aztreonam, ceftazidime, piperacillin/tazobactam and resistant to amikacin, cefepime, ciprofloxacin, gentamicin, levofloxacin, meropenem and tobramycin, by the Kirby Bauer method.
Case Follow Up
The patient was ultimately treated with IV piperacillin/tazobactam, as well as with chest physical therapy and hypertonic saline inhalation. They clinically improved and were ultimately discharged home after a 2 week hospital stay.
References
The mucoid switch in Pseudomonas aeruginosa represses quorum sensing systems and leads to complex changes to stationary phase virulence factor regulation. Ben Ryall, Marta Carrara, James EA Zlosnik, Volker Behrends, Xiaoyun Lee, Zhen Wong, Kathryn E. Lougheed, Huw D. Williams. PLOS ONE, May 2014, Vol. 9, Iss. 5, Pages 1-11.
Pseudomonas aeruginosa biofilms in cystic fibrosis. Niels Høiby, Oana Ciofu, and Thomas Bjarnsholt. Future Microbiology, November 2010, Vol. 5, No. 11, Pages 1663-1674.
Insights into Cystic Fibrosis Polymicrobial Consortia: The Role of Species Interactions in Biofilm Development, Phenotype, and Response to In-Use Antibiotics. Magalhaes AP, Lopes SP, Pereira MO. Frontiers in Microbiology, January 13, 2017, Vol. 7, Article 2146.
Koneman’s Color Atlas and Textbook of Diagnostic Microbiology. Gary W. Procop, Deirdre L. Church, Geraldine S. Hall, William M. Janda, Elmer W. Koneman, Paul C. Schreckenberger; Gail L. Woods. Seventh Edition. 2017. Pages 343, 1110.

-Megan B. Wachsmann, MD, MSCS, is a 4th year Anatomic and Clinical Pathology Resident and Chief Resident at UT Southwestern Medical Center.

–Erin McElvania TeKippe, PhD, D(ABMM), is the Director of Clinical Microbiology at Children’s Medical Center in Dallas Texas and an Assistant Professor of Pathology and Pediatrics at University of Texas Southwestern Medical Center.
