Case History
After experiencing increasingly frequent asthma attacks and multiple episodes of pneumonia within the last two years, a 60 year-old woman with a longstanding history of allergic asthma presents to a pulmonologist complaining of increased shortness of breath and cough. The patient reports a history of abnormal lung infiltrates for which she was previously treated with a three month course of azithromycin. A repeat chest CT shows diffusely scattered, nodular, ground-glass opacities which have increased in number since her last CT two year prior. A bronchoalveolar lavage is performed and specimen is sent for bacterial, fungal, and AFB cultures as well as a respiratory virus PCR panel.
Laboratory Identification
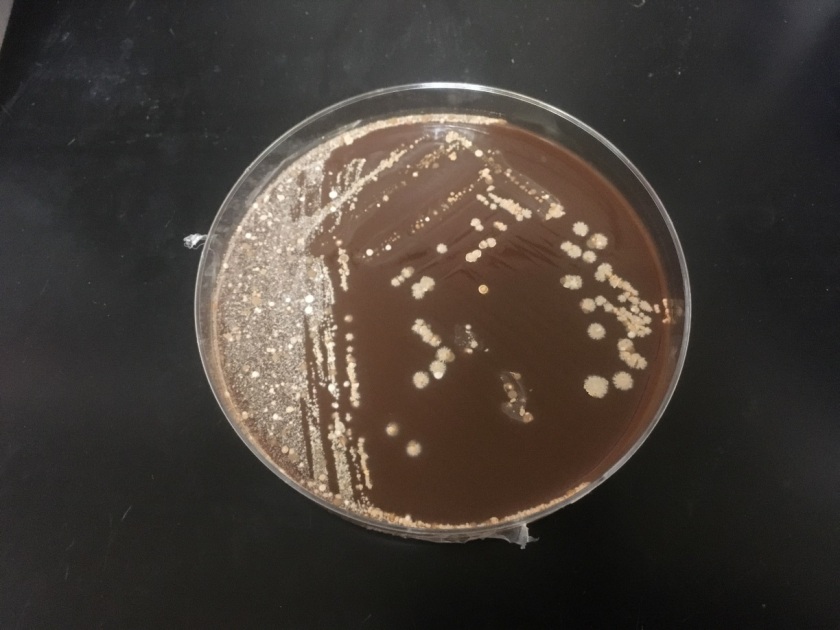
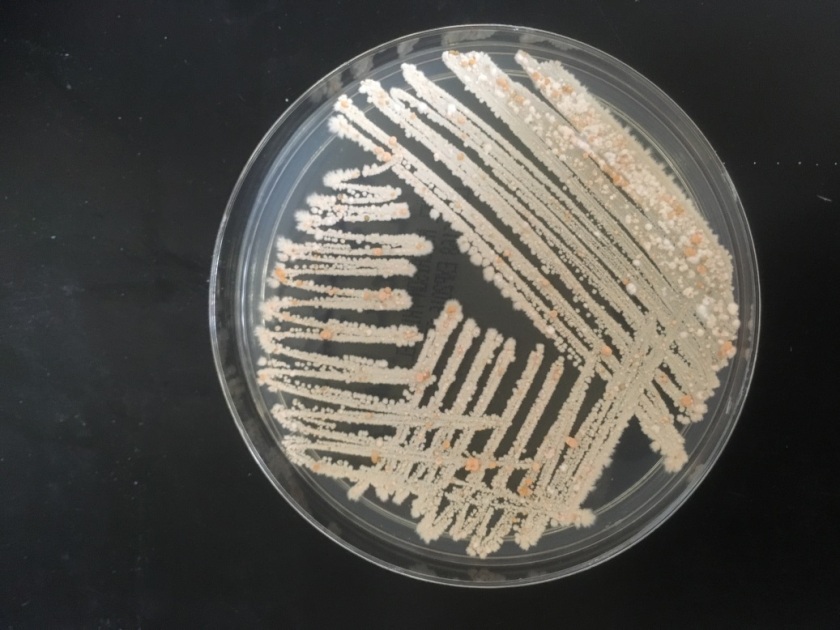
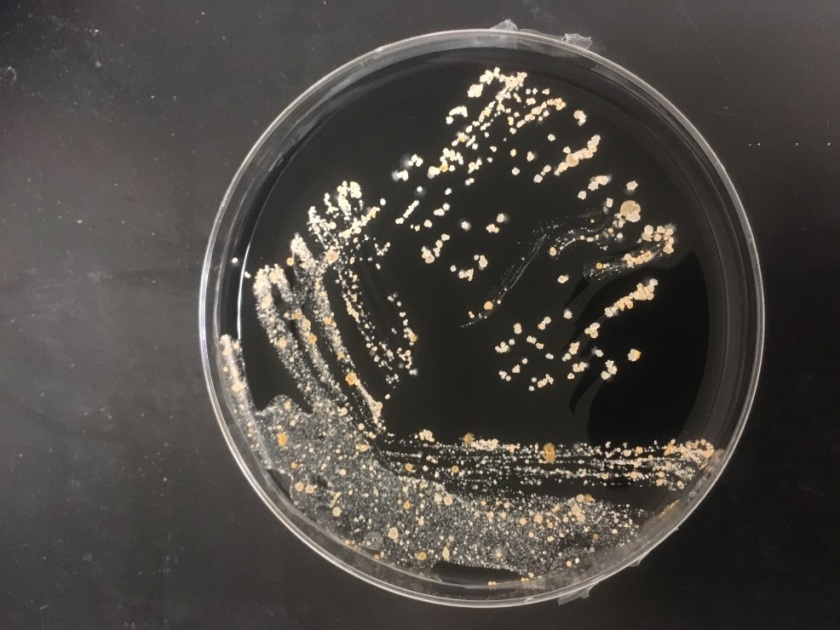
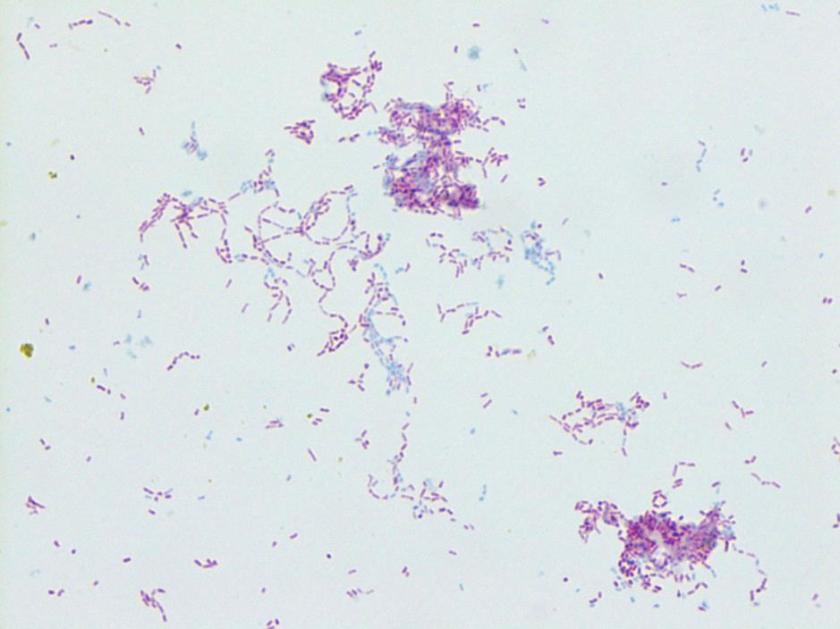
The bacterial and fungal cultures do not grow any pathogens and the respiratory virus panel is negative. The AFB culture, however, grows beaded, Gram-Positive bacilli which are Auramine/Rhodamine negative and Modified Kinyoun positive. The organism grows well on 7H11, Chocolate, and Buffered Charcoal Yeast Extract (BCYE) agars forming irregular, chalky, white-pink colonies.
The organism is confirmed as Nocardia nova by molecular methods.
Discussion
Nocardia nova is a ubiquitous soil bacteria and one of several Nocardia species known to cause disease in humans. When contracted through traumatic inoculation, Nocardia may cause cutaneous diseases such as a mycetoma, superficial abscesses, or cellulitis. More commonly, however, Nocardia is contracted via inhalation and presents as a chronic, slowly progressive pulmonary infection with cough, shortness of breath, and fever. Complicated pulmonary infections may result in pleural effusions, empyema, pericarditis, chest wall abscesses, or dissemination to the brain and other deep organs. Due to low virulence, Nocardia primarily affects only the immunocompromised but those with pre-existing pulmonary disease are also susceptible to infection.
Nocardia is identified in the laboratory as an aerobic filamentous, beaded, Gram-Positive bacilli demonstrating right-angled branching. Nocardia is also weakly acid-fast and is usually identified by a Modified Kinyoun stain. While Nocardia grows within 3-5 days on blood and chocolate agar, it is often isolated on mycobacterial media or BCYE plates where it forms chalky white to faintly pigmented colonies. Accurate identification and speciation of Nocardia currently requires the use of molecular methods (primarily 16S ribosomal RNA gene sequencing). While many infections are successfully treated with a sulfonamide for 6 months to 1 year, the CDC recommends performing speciation and anti-microbial susceptibility testing on every clinical isolate due to species specific susceptibility profiles and multi-drug resistant strains. Nocardia farcinica, for example, is resistant to many antibiotics including 3rd generation cephalosporins.
-Elaine Amoresano, MD, is a 2nd year anatomic and clinical pathology resident at the University of Vermont Medical Center.

-Christi Wojewoda, MD, is the Director of Clinical Microbiology at the University of Vermont Medical Center and an Assistant Professor at the University of Vermont.

Good case.
VERY INTERESTING